Today, I review, link to, and excerpt from the Obesity Association‘s “Pharmacologic Treatment of Obesity in Adults: Standards of Care in Overweight and Obesity”. [PubMed Abstract] [Full-Text HTML] [Full-Text PDF]. BMJ Open Diabetes Res Care. 2026 Jan 13;13(Suppl 1):e005729. doi: 10.1136/bmjdrc-2025-005729.
All that follows is from the above resource
Abstract
Obesity medications may be part of a comprehensive care plan for adults with obesity. The Obesity Association, a division of the American Diabetes Association (ADA), developed comprehensive, evidence-based guidelines on the pharmacologic treatment of obesity in adults. When used in conjunction with lifestyle modifications, obesity medications have demonstrated efficacy in inducing and sustaining weight reduction while concurrently improving clinical outcomes of obesity and obesity-related diseases and complications. Healthcare professionals should engage people with obesity in a person-centered, shared decision-making approach when selecting an obesity medication to optimize health outcomes while emphasizing individual needs and preferences. The ADA’s Obesity Association encourages healthcare professionals to adopt these guidelines for treatment of obesity in adults.
Keywords: Drug Therapy; Obesity; Pharmacology; Practice Guideline.
© 2026, American Diabetes Association, Inc., and BMJ Publishing Group Limited.
Obesity medications are an essential component of a
comprehensive approach to obesity management, offering significant benefits beyond lifestyle interventions
alone for many people. Research indicates that pharmacotherapy can lead to greater weight reduction and improved weight maintenance than placebo in adults with
obesity (1). Of note, randomized controlled trials (RCTs)
of obesity medications include lifestyle intervention in
both placebo and study drug arms, which most typically comprises a 500-calorie deficit meal plan and behavioral intervention that usually produces 2.6% weight
reduction in the placebo group (2), and the placebo
group receives a placebo pill or injection, as appropriate. In meta-analyses of RCTs, people treated with obesity medications experienced substantial weight
reduction compared with placebo (2,3). Participants
treated with obesity medications also had improvements
in cardiometabolic markers, such as glycemia and lipid profiles (2,3), and some obesity medications demonstrated
improvements in cardiovascular outcomes and other obesity-related diseases (4–7). When used appropriately, obesity medications offer a favorable risk-benefit profile in
many cases, making them a viable option for many people
with obesity.As obesity medications induce clinically meaningful
weight reduction relative to placebo (2,18), the choice of
therapy should prioritize medications most likely to improve obesity-related diseases and complications and to
achieve and maintain weight reduction goals. Therefore,
this section outlines an approach focused on reducing
risk of and burden from obesity-related diseases rather
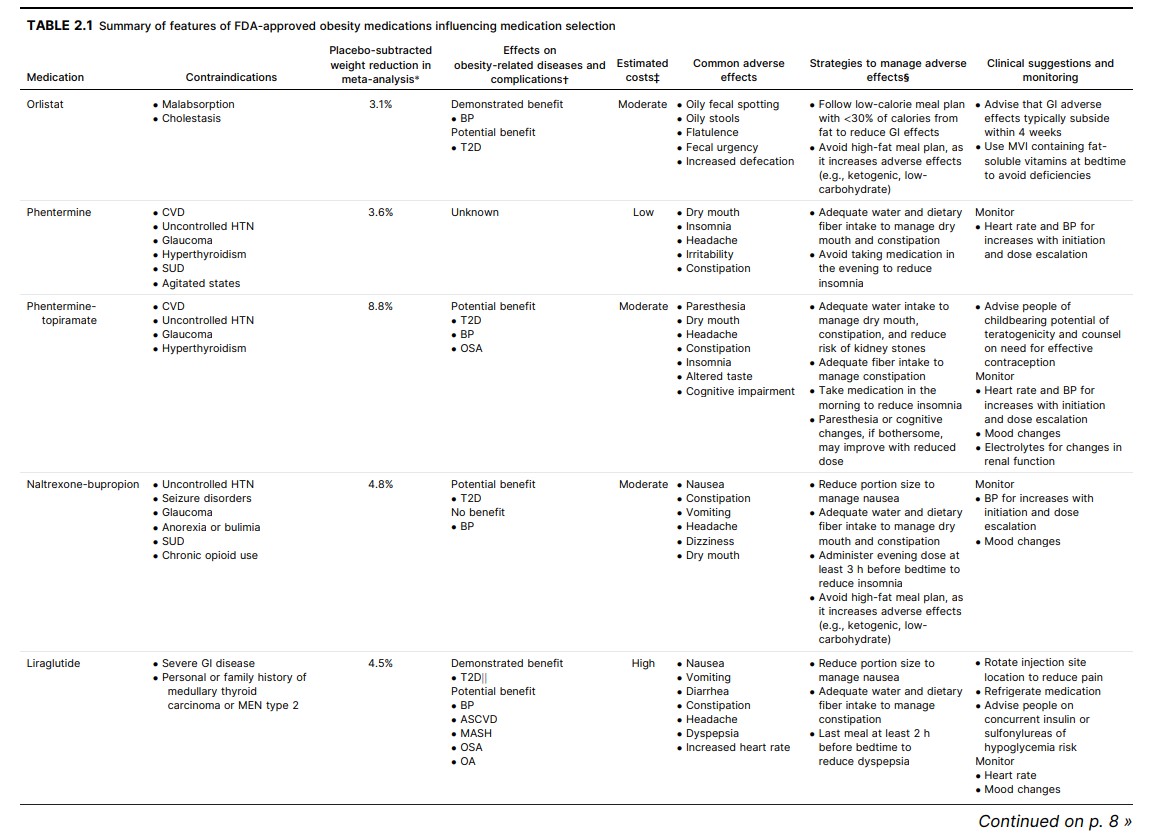
than solely focusing on weight reduction goals. Table 2.1
contains a summary of treatment and weight-reduction
outcomes as well as adverse effects reported in RCTs of
obesity medications. The risk of medication-related adverse effects should be evaluated for each individual, as
this risk may vary depending on their medical history and
concomitant medications. In a network meta-analysis
(132 RCTs), adverse events leading to drug discontinuation were significantly higher for all obesity medications
compared with placebo (2). Health care professionals
should present the potential benefits, risks, and expected
outcomes of obesity medications. Medication selection
should be guided by person-centered factors, including evidence, treatment burden, costs, and individuals’ therapeutic
goals and preferences.Behavioral Lifestyle Therapy With Obesity
MedicationsNutrition, physical activity, and behavioral therapy must be
components of all comprehensive obesity treatment plans,
including those with obesity medications. The efficacy of
obesity treatment interventions that include nutrition and
physical activity have been documented in meta-analyses
(1,19,20), and the addition of obesity medications to lifestyle
interventions improves weight reduction and weight loss
maintenance (1,19,21).
Greater weight reduction may be achieved when a lifestyle
behavioral modification program is administered with an
obesity medication among individuals with obesity (22–25).
For example, in a 1-year RCT, participants in a naltrexonebupropion plus intensive behavioral program group lost
9.3% of baseline weight compared with 5.1% in the placebo
plus intensive behavioral program group (22). The degree of
weight reduction achieved is related to program intensity
(20), and engagement in behavioral components is also associated with greater weight reduction (26). Some obesity
medications are associated with increased fullness as well
as decreased hunger, food preoccupation, dietary disinhibition, and binge eating compared with placebo (27,28),
which may aid individuals in achieving and sustaining the
lifestyle treatment plan.Weight-Promoting Medications
Before prescribing an obesity medication, health care professionals should carefully review individuals’ concomitant
medications, as studies have found that medications
that promote weight gain are commonly used, including
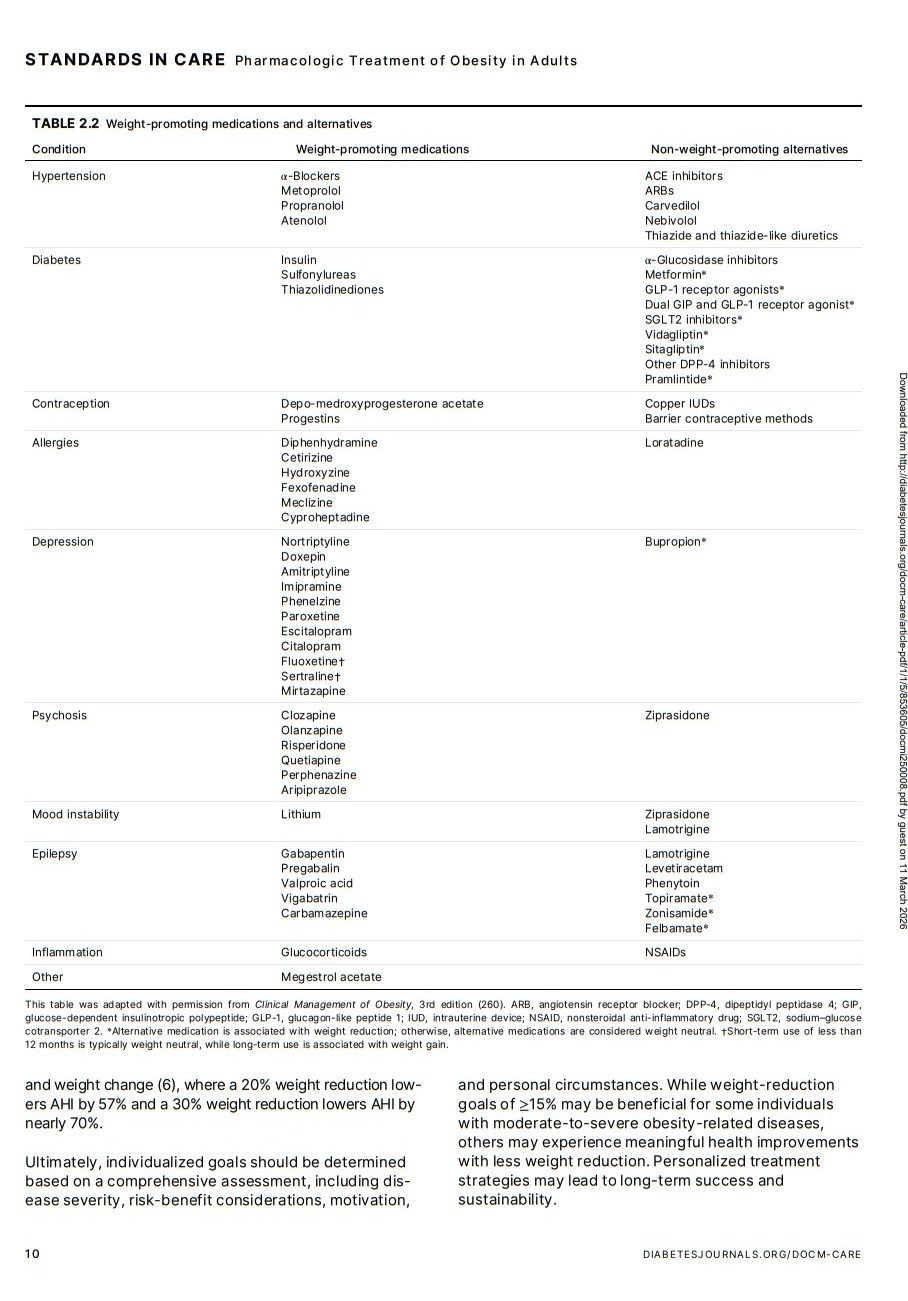
among individuals with obesity (29–31). Health care professionals should be aware of weight-promoting medications (Table 2.2) (32). As the number of prescribed
weight-promoting medications increases, individuals’
BMI and waist circumference are more likely to have
greater increases over time (33). In addition, studies
have found that participants using weight-promoting
medications have reduced weight loss efficacy with lifestyle interventions to treat obesity (34,35).Whenever possible and clinically appropriate, avoid initiating
a prescription for weight-promoting medications among
individuals with obesity and instead select a non-weightpromoting alternative. For example, ACE inhibitors, angiotensin receptor blockers, calcium channel blockers, and
diuretics should be prioritized to treat hypertension rather
than some β-blockers, as these options are weight-neutral
rather than weight-promoting. When diabetes medications
are needed for glycemic management, medications most
likely to cause weight gain should be discouraged in favor
of alternatives that are non-weight-promoting (Table 2.2).
However, health care professionals should not refrain from
prescribing weight-promoting medications when needed to
achieve treatment goals for that condition (e.g., blood pressure in hypertension).
For individuals with obesity who may already be using
weight-promoting medications, health care professionals
should determine whether a dose reduction or nonweight-promoting alternative may be clinically appropriate. If so, individuals should be engaged in determining
whether their medication plan should be modified, accounting for the benefits and risks of all treatment options.
Health care professionals should be aware that cessation
of weight-promoting medications does not necessarily result in weight reduction. For individuals who must remain
on weight-promoting medications, obesity medications
may be beneficial in achieving treatment and weight goals.Setting Treatment Goals With Obesity
MedicationsAchieving a ≥5% reduction in baseline body weight for
adults treated with obesity medications is associated with
health benefits (18,38–42). Research demonstrates that a
5% weight reduction improves cardiometabolic risk factors
(2,43,44). For example, the CONQUER RCT demonstrated
that over 60% of participants treated with phenterminetopiramate achieved ≥5% weight reduction as compared with 21% with placebo, and weight reduction was accompanied by improvements in metabolic risk factors (40). In
the SURMOUNT-1 RCT, over 85% of participants who received tirzepatide achieved a ≥5% reduction goal compared with 35% with placebo; notable improvements in
cardiometabolic measures were also observed (18).For individuals with obesity-related diseases and complications, achieving ≥10% reduction in baseline body weight
has consistently demonstrated improvements in these
conditions. In general, 10–15% weight reduction results in
significantly greater improvements in glycemia, blood
pressure, and lipids compared with 5–10% loss (45). In
most cases, the magnitude of weight reduction is directly
proportional to risk factor improvements; therefore, sustained weight reduction of ≥10% is often required for optimal
cardiometabolic benefits. Obesity-related diseases and conditions that benefit from this weight loss magnitude include
metabolic dysfunction–associated steatohepatitis with moderate-to-severe fibrosis (7,46), heart failure with preserved
ejection fraction (47,48), and knee osteoarthritis (49).Emerging data suggest that ≥15% weight reduction may be
needed to achieve clinical benefits in some cases (45), particularly for individuals with moderate-to-severe obesityrelated conditions. In the SURMOUNT-OSA trial, participants with obesity and moderate-to-severe obstructive sleep apnea who received tirzepatide achieved mean weight reduction exceeding 15% and experienced significant reductions
in the apnea-hypopnea index (AHI), hypoxic burden, and
systolic blood pressure compared with placebo (6). A metaanalysis found a dose-response relationship between AHI and weight change (6), where a 20% weight reduction lowers AHI by 57% and a 30% weight reduction lowers AHI by
nearly 70%.Ultimately, individualized goals should be determined
based on a comprehensive assessment, including disease severity, risk-benefit considerations, motivation,
and personal circumstances. While weight-reduction
goals of ≥15% may be beneficial for some individuals
with moderate-to-severe obesity-related diseases,
others may experience meaningful health improvements
with less weight reduction. Personalized treatment
strategies may lead to long-term success and
sustainability.Selecting Obesity Medications