5.3. Laboratory Measurement (continued)
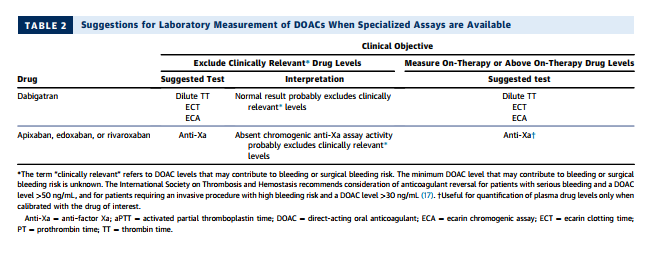
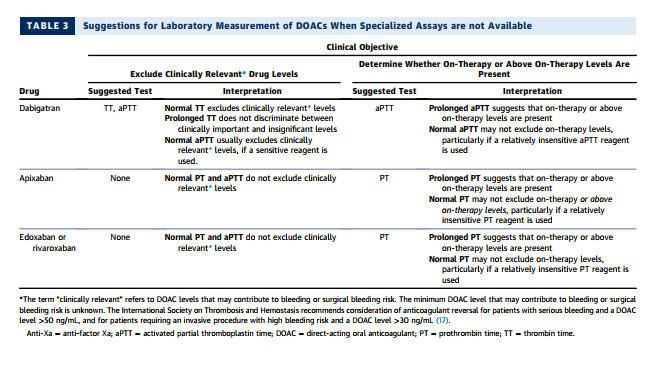
The best tests for assessing the anticoagulant activity of dabigatran include the dilute thrombin time, ecarin clotting time, and ecarin chromogenic assay (see Table 2) (18,19). These tests correlate closely with dabigatran levels measured by the reference standard method, liquid chromatography-tandem mass spectrometry. Unfortunately, these assays are not widely available, particularly on an emergent basis (18,19). In their absence, the thrombin time (TT) and aPTT may be used for qualitative assessment (see Table 3). The TT is exquisitely sensitive to dabigatran, even at very low drug concentrations. Thus, a normal TT excludes clinically relevant dabigatran levels, but a prolonged TT does not discriminate between clinically important and insignificant drug concentrations. All laboratories that do not offer an around-theclock assay for dabigatran quantification should be encouraged to offer the TT for rapid exclusion of clinically significant dabigatran levels. A prolonged aPTT suggests the presence of on-therapy or above on-therapy levels of dabigatran. However, a normal aPTT does not exclude the presence of on-therapy levels, especially when a relatively insensitive aPTT reagent is used (16,18,19)
The preferred test for assessing the anticoagulant activity of apixaban, edoxaban, and rivaroxaban is a chromogenic anti-Xa assay (see Table 2) (18,19). When the assay is calibrated with the drug of interest, the results correlate closely with plasma drug levels measured by liquid chromatography-tandem mass spectrometry. When the assay is calibrated with a low-molecular-weight heparin standard, it can be useful for excluding clinically important levels of drug, but not for quantitation. If an anti-Xa assay is not available, the PT may be useful for qualitative assessment of edoxaban and rivaroxaban. A prolonged PT suggests on-therapy or above on-therapy levels for these agents. However, depending on the sensitivity of the PT reagent, a normal PT may not exclude on-therapy levels (18,19). The PT and aPTT are insensitive to apixaban. A prolonged PT suggests the presence of clinically important apixaban levels, but a normal PT and aPTT do not exclude on-therapy or even above on-therapy levels of the drug (18–20).
Follow Tom On:
Categories
-
Recent Posts
- Linking To And Excerpting From The CDC’s “Diagnosing Tuberculosis”
- Linking To And Embedding Metabolic Mind And Georgia Ede MD’s “Fell Out of Ketosis? Here’s How to Get Back Fast”
- Linking To And Embedding Metabolic Mind’s “Bounce Back Stronger: Dr. Matt Bernstein on Mental Health Setbacks”
- Susan Schneider Williams, Robin Williams’ Wife, Shares The Tragic Story Of His Death From Lewy Body Dementia
- Linking To And Embedding Metabolic Mind And Georgia Ede MD’s “Go Slowly: A Beginners Guide to Psychiatric Drug Tapering (Part 2)”
- Linking To And Embedding Metabolic Mind And Georgia Ede MD’s “Taper Down Slowly: A Beginners Guide to Psychiatric Drug Tapering (Part 1)”
- Linking To And Excerpting From JN Learning’s “Transcript PrEP Prevents HIV—If Patients Can Get It”
- Linking To And Embedding Metabolic Mind’s “Depression and Metabolism: What This New Study Reveals” (And How To Establish A Virtual Ketogenic Diet Clinic)
- Linking To And Embedding CriticalCareNow’s “Ultrasound In Peri-Arrest”
- Linking To And Excerpting The 2026 ACC/AHA Lipid Management Guidelines “What’s New”T
- Linking To The ACC/AHA 2026 Lipid Management Guidelines “Top (10) Take Home Messages”
- Linking To And Excerpting From “2026 ACC/AHA/AACVPR/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA Guideline on the Management of Dyslipidemia: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines”
- Links To The American Heart Association’s “CPR And ECG Guidelines”-2025
- Outstanding: YouTube Video “Ultrasound In Cardiac Arrest” From MetroHealth Emergency Ultrasound
- Linking To And Excerpting From Clinical Insights In Eye Care’s “A Case Report: Diagnosing Arteritic Anterior Ischemic Optic Neuropathy Secondary to Giant Cell Arteritis”
- Linking To And Embedding Doctor Eye Health’s “GLP 1 Blindness Risk | Should You Be Worried?”
- Linking To And Excerpting From The Liver Fellow Network’s “How to approach elevated liver enzymes?”
- Linking To And Embedding NeoPocusCollab’s “Targeted Use of POCUS for a Crashing Infant in the NICU: SAFE-R Protocol”
- Linking To And Excerpting From “Pharmacologic Treatment of Obesity in Adults: Standards of Care in Overweight and Obesity”
- Linking To Resources From The Obesity Association Of The American Diabetes Association
- Posting Liver Fellow Network’s Outstanding “Back to Basics: Liver Associated Enzymes” Infographic
- Linking To And Excerpting From StatPearls’ “Liver Imaging” With Additional Links
- Linking To And Excerpting From The New York Times Article “Take It From a Doctor: It’s OK if Your Medical Advice Comes From A.I.”
- Linking To And Embedding Metabolic Mind’s “The Hidden Metabolic Cause of Fatty Liver Disease” With Additional Resources
- Linking To And Embedding EM Note’s “Euglycemic DKA”
- Linking To CORE IM’s “Which IV should you use?” [Links To Two Videos And The Transcript]
- Linking To And Excerpting From Nutrients’ “The Ketogenic Diet in Type 2 Diabetes and Obesity: A Narrative Review of Clinical Evidence”
- Dr. Sam’s Playlist “Ultrasound Probe Positioning” (22 Videos)
- Substack’s Playlist “Podcasting On Substack” (10 Videos)
- Linking To CORE IM’s “Which IV should you use?” [Infographics]