The following are from Sections 10 and 10.2 [pp 923 + 924] from the 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure:
10. Arrhythmias and conductance disturbances
Ambulatory electrocardiographic monitoring can be used to investigate symptoms that may be due to arrhythmias,322 – 324but evidence is lacking to support routine, systematic monitoring for all patients with HF to identify tachy- and bradyarrhythmias. There is no evidence that clinical decisions based on routine ambulatory electrocardiographic monitoring improve outcomes for patients with HF. Ambulatory electrocardiographic recording detects premature ventricular complexes in virtually all patients with HF. Episodes of asymptomatic, non-sustained VT are common, increasing in frequency with the severity of HF and ventricular dysfunction and indicating a poor prognosis in patients with HF, but provide little discrimination between sudden death or death due to progressive HF.316,325 Bradycardia and pauses are also commonly observed, especially at night when sympathetic activity is often lower and para-sympathetic activity higher; sleep apnoea may be a trigger.326 – 328 Pauses are associated with a poor prognosis in patients with CAD and left ventricular dysfunction.329 Bradyarrhythmias may make an important contribution to sudden death in heart failure.
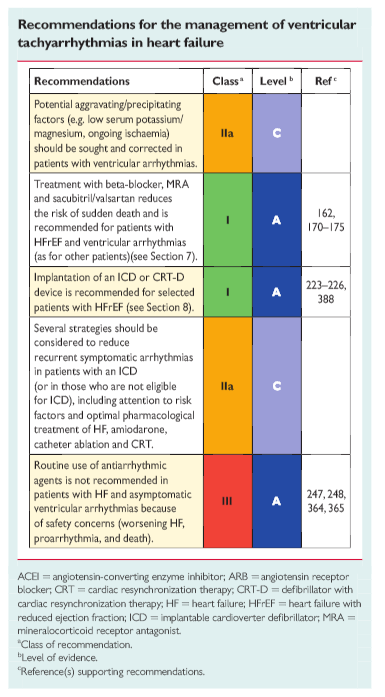
10.2 Ventricular Arrythmias [What follows is the complete text of 10.2]
The initial management of asymptomatic ventricular arrhythmiasis correction of electrolyte abnormalities, particularly low serum potassium and magnesium, withdrawal of agents that migh tprovoke arrhythmias and, in patients with HFrEF, optimization of pharmacological therapy with ACEIs, beta-blockers and MRAs and sacubitril/valsartan, which all reduce the risk of sudden death.174,177,383,384
The clinical relevance of myocardial ischaemia for the provocation of ventricular arrhythmias is uncertain, although anecdotal cases of ischaemia-induced arrhythmias exist. Randomized trials of revascularization for patients with HFrEF have not reduced overallmortality,107,385even in subgroups of patients with angina or myo-cardial ischaemia,115,386but further analysis did suggest a reduction in sudden deaths.38
Amiodarone (often in combination with a beta-blocker) may beused to suppress symptomatic ventricular arrhythmias, but it mayadversely affect prognosis, especially in patients with more severeHF.227,244Other antiarrhythmic drugs should be avoided.247Trans-catheter radiofrequency modification of the arrhythmogenic sub-strate may reduce the number of appropriate ICD dischargesand may be used to terminate arrhythmic storm in patients with HF and frequent, recurrent ventricular tachyarrhythmias andtherefore should be considered in such patients. Seeking the advice of the members of the HF Team with expertise in electro-physiology is recommended in patients with recalcitrant ventricular arrhythmias. For further details we refer the reader to the ESC/EHRA guidelines on ventricular arrhythmias and sudden cardiac death.260 [Links to this guideline is in Resource (3) below]
Resources:
(1) 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. [PubMed Citation] [Full Text HTML] [Full Text PDF]. Eur J Heart Fail. 2016 Aug;18(8):891-975. doi: 10.1002/ejhf.592. Epub 2016 May 20.
(2) 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart
failure – Web Addenda [Full Text PDF -you may need t register for a free ESC account to access this resource]
(3) 2015 ESC Guidelines for the management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: The Task Force for the Management of Patients with Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death of the European Society of Cardiology (ESC). Endorsed by: Association for European Paediatric and Congenital Cardiology (AEPC) [PubMed Abstract] [Full Text HTML] [Full Text PDF]. Eur Heart J. 2015 Nov 1;36(41):2793-867. doi: 10.1093/eurheartj/ehv316. Epub 2015 Aug 29.