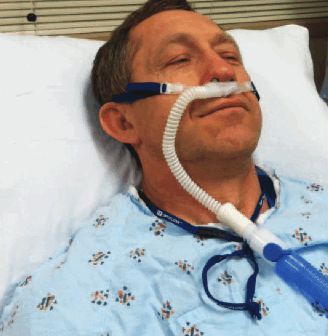
What follows are some excerpts from Dr. Farkas’ Pulcrit post “High-flow nasal cannula to prevent post-extubation respiratory failure of July 16, 2014:
Background: Post-extubation failure and noninvasive ventilation (NIV)
Post-extubation respiratory failure requiring re-intubation is a major setback for any critically ill patient. Current evidence mainly involves the pre-emptive use of NIV to reduce post-extubation failure, particularly in hypercapnic COPD patients. However, in practice this is difficult to implement widely. Except for the sickest COPD patients, it’s often difficult to persuade the patient to continue NIV long enough to benefit. Many patients with respiratory failure aren’t ill enough to justify NIV, yet remain at risk for extubation failure. Some patients have contraindications to NIV.
Physiology of post-extubation respiratory failure and role of pre-emptive ventilatory support
The most common cause of post-extubation respiratory failure is inability of the respiratory muscles to sustain the work of breathing, leading to progressive muscle fatigue (figure below). The first sign of decompensation is usually a gradually rising respiratory rate (a rapid-shallow breathing pattern is the body’s compensatory response to an excessive work of breathing). Based on this model, when evaluating an intervention to avoid reintubation the key variables pay attention to are respiratory rate and carbon dioxide tension (not oxygenation)
And there is good evidence that we can follow carbon dioxide tension with a venous blood gas instead of having to use an arterial blood gas. See Resource (1) below.
It’s important to differentiate between pre-emptive respiratory support (initiated at time of extubation) vs. salvage support (initiated later on, when the patient develops respiratory failure). NIV is only shown to be effective for pre-emptive support. This makes sense. Post-extubation failure is usually due to excessive work of breathing, with accumulating respiratory muscle fatigue. By the time the patient becomes significantly dyspneic, the respiratory muscles may already be fatigued and it may be too late to intervene.
Conclusions
One of the primary goals of critical care is to safely and efficiently liberate patients from mechanical ventilation. Post-extubation respiratory failure requiring reintubation is a huge setback, and any way to avoid this is very welcome. HFNC is emerging as a safe and well-tolerated approach to support a patient’s oxygenation and ventilation. Maruzio et al. suggests that initiation of HFNC immediately following extubation reduces the risk of reintubation. Currently, post-extubation NIV is supported by a much greater body of evidence, and remains the first-line approach when indicated. For patients who aren’t candidates for post-extubation NIV or who are unable to tolerate NIV, HFNC may be an attractive option. For maximal efficacy, the flow rate should probably be kept high (i.e., 40-50 liters/minute) to reduce the work of breathing.
Resources
(1) Correlation of Venous Blood Gas and Pulse Oximetry With Arterial Blood Gas in the Undifferentiated Critically Ill Patient [PubMed Abstract] [Full Text HTML] [Full Text PDF]. J Intensive Care Med. 2018 Mar;33(3):176-181. doi: 10.1177/0885066616652597. Epub 2016 Jun 9.
(2) PulmCrit- Mastering the dark arts of BiPAP & HFNC, February 12, 2018 by Dr. Farkas
(3) High-flow nasal cannula to prevent post-extubation respiratory failure
July 16, 2014 by Josh Farkas
(4) High-flow nasal oxygen therapy in intensive care and anaesthesia [PubMed Abstract] Full Text HTML] [Full Text PDF]. Br J Anaesth. 2018 Jan;120(1):18-27. doi: 10.1016/j.bja.2017.11.010. Epub 2017 Nov 21.
(5) PulmCrit – Optimizing the respiratory drive to avoid failure, December 4, 2017 by Dr. Josh Farkas.
(6) Pneumonia, BiPAP, secretions, and HFNC: New lessons from FLORALI
May 25, 2015 by Dr. Josh Farkas.
(7) PulmCrit- Top 10 reasons pulse oximetry beats ABG for assessing oxygenation
November 2, 2016 by Dr. Josh Farkas.