What follows is from Resource (1) below.
The assessment of COPD must consider four aspects:
- The presence and severity of spirometric abnormalities
- The current nature and magnitude of the patient’s symptoms
- Exacerbation history and future risks
- Presence of comorbidities
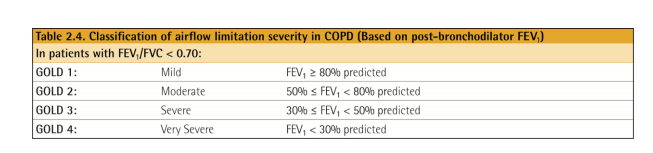
Spirometric abnormalities:
GOLD states (p 31, 47 of the PDF):
It should be noted that there is only a weak correlation between FEV1 symptoms and impairment of a patient’s health status. For this reason, formal symptomatic assessment is required.
Assessment of Symptoms
Because COPD impacts the patient’s health status beyond just dyspnea, GOLD 2017 recommends a comprehensive assessment of symptoms rather than just a measure of dyspnea such as the mMRC dyspnea scale.
The most comprehensive disease specific symptom scores are the Chronic Respiratory Questionnaire (CRQ) and St. George’s Respiratory Questionnaire. But GOLD 2017 states that they are too complex to be used in routine practice.
Instead, Gold recommends use of the COPD Assessment Test (CAT) and the COPD Control Questionnaire.
GOLD 2017 recommends treating stable patients with COPD based on symptom reports rather than on spirometry.
However, GOLD notes (p 32 -48 of PDF):
The CAT and the CCQ provides measures of symptomatic impact of COPD but does not categorize patients into symptom severity groups for the purpose of treatment.
It is not clear to me how one can treat the symptoms of COPD with expensive inhalers if the symptom score you use is not designed to measure clinically meaninful changes in symptoms.
For more on symptom scores see my post with references Symptom Scores For Monitoring COPD Posted on July 19, 2017
Assessment Of Acute Exacerbation Risk
GOLD 2017 on p 33 (49 of the PDF) states:
COPD exacerbations are defined as an acute worsening of respiratory symptoms that result in additional therapy. These events are classified as mild (treated with short acting bronchodilator (SABDs) only), moderate (treated with SABDs plus antibiotics and/or oral corticosteroids) or severe (patient requires hospitalization or visits the emergency room). Severe exacerbations may also be associated with acute respiratory failure. A number of large studies including patients classified using Gold’s parametric grading systems have been conducted and showed that the rate at which exacerbations occur varies greatly between patients. The best predictor of having frequent exacerbations (defined as two or more exacerbations per year) is a history of earlier treated events.
In addition, deteriorating airflow limitation is associated with an increased prevalence of exacerbations hospitalizations, and risk of death. Hospitalization or a COPD exacerbation is associated were prognosis increased risk of death. There is also a significant relationship severity and risk of exacerbation and death. At the population level approximately 20% gold to (moderate airflow limitation) patients may. Exacerbations require treatment with antibiotics and or systemic records there. The risk of exacerbations significantly higher Asian with gold three (severe) and gold for (very severe). However, FEV1 by itself lacks sufficient precision (i.e., wide variation) to be used clinically as a predictor of exacerbations or mortality in patients with COPD.
Assessment of concomitant chronic diseases (comorbidities)
GOLD 2017 on p 33 (49 of the PDF) states:
Patients with COPD often have important concomitant chronic illnesses at the time of diagnosis and COPD represents an important component of multi-morbidity development particularly in the elderly in response to common risk factors (e.g., aging, smoking, alcohol, diet and inactivity). . . .
Common comorbidities include cardiovascular disease, skeletal muscle dysfunction, metabolic syndrome, osteoporosis, depression, anxiety and lung cancer. The existence of COPD may actually increase the risk for other diseases; this is particularly striking for COPD and lung cancer. Whether this association is due to the risk factors (e.g., smoking), involvement of susceptibility genes, or in scared clearance of carcinogens is not clear.
Comorbidities can occur in patients with mild, moderate, and severe airflow limitation, influence mortality independently, and deserve specific treatment. Therefore, comorbidities should be looked for routinely and treated appropriately in any patient with COPD. Recommendations for the diagnosis, assessment of severity, and management of comorbidities in patients with COPD are the same as for all other patients. A more detailed assessment of COPD and comorbidities is provided in Chapter 6 [pp 114 – 123 (pp 130 – 139 of the PDF)].
Revised combined COPD assessment
GOLD 2017 on p 34 – 36 (pp 50 – 52 of the PDF):
There are three aspects to COPD assessment: the spirometry grade based on the FEV1 (see table above) and the ABCD symptom assessment tool, and finally the number of exacerbations.
A symptom score:
An mMRC of 0 -1 or a CAT of < 10 and
An exacerbation history of 0 – 1 (not leading to hospitalization)
B symptom score:
An mMRC of >/= 2 or a CAT of >/= 10 and
An exacerbation history of 0 – 1 (not leading to hospitalization)
C symptom score:
An mMRC of 0 -1 or a CAT of < 10 and
An exacerbation history of >/= 2 or >/= 1 leading to hospital admission
D symtom score:
An mMRC of >/= 2 or a CAT of >/= 10 and
An exacerbation history of >/= 2 or >/= 1 leading to hospital admission
Note: In cases where there is a marked discordance between the level of airflow and the perceived symptoms, a more detailed evaluation should be carried out to better understand the mechanics (e.g., full lung function tests), lung structure (e.g., computed tomography) and or comorbidities (e.g., ischemic heart disease) that might impact patient symptoms. In some cases patients may endorse minimal symptoms despite demonstrating severe airflow limitation. Adapting to the limitations imposed by COPD, these patients may reduce their level of physical activity in a way that may result in an underestimation of symptom load. Exercise tests like the six minute walking test distance may reveal that the patients are severely constrained and do need more intense treatment.
Neither spirometry nor the ABCD symptom tool is better “for mortality prediction or other important health outcomes in COPD.”
For COPD prognostication please see my post Determining Prognosis In COPD – The BODE Index. Posted on July 12, 2017
Resources:
(1) The Global Initiative For Chronic Obstructive Lung Disease has published GOLD 2017 Global Strategy for the Diagnosis, Management and Prevention of COPD[Download link to PDF] and the POCKET GUIDE TO COPD DIAGNOSIS, MANAGEMENT, AND PREVENTION: A Guide for Health Care Professionals 2017 REPORT [Link is to the PDF]