This blog and the posts on it are my study notes which I put up to help me reinforce my learning on the subjects I review.
I’m reviewing all of the excellent diagnostic schemas from the Clinical Problem Solvers.
And today I review the diagnostic schema Hypercalcemia [This link is to the web page where the video of the schema is discussed. Be sure to review the video].
Here are the links to the Hypercalcemia podcasts:
Here is the diagnostic schema [Link is to the PDF] and after the diagnostic schema below I have placed a copy of the show notes for Episodes 7 and 8 [Link is to the PDF]:
Show Notes For Episodes 7 & 8
This week, the CPSers introduce a schema for hypercalcemia in Episode 7 and then apply it to an fascinating unknown case from guest Dr. Bob Centor in Episode 8.
Problem Representation – episode 8
Dr. Centor presented the case of a 50-year-old man with a history of Crohn’s disease treated with a total colectomy who presented with subacute increased ileal output, tachycardia, and
hypercalcemia.Schemas
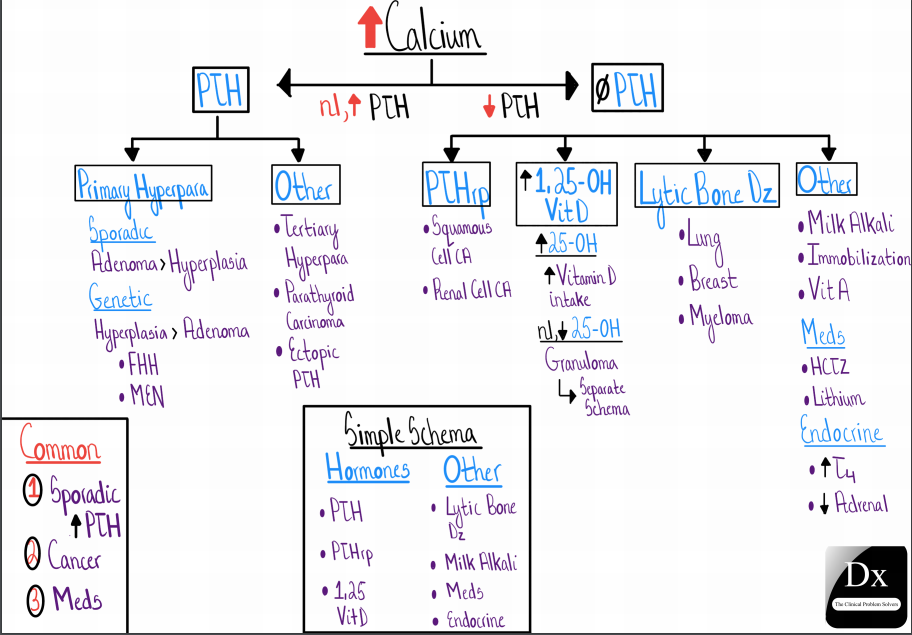
The CPSers’ schema for hypercalcemia classifies the causes into PTH and non-PTH mediated etiologies.Diagnosis – episode 8
They eventually cracked the case when thyroid studies confirmed a diagnosis of hyperthyroidism – a rare cause of hypercalcemia!Teaching points
• The combination of constipation and polyuria is much more specific for hypercalcemia than classically described symptoms (bones, stones, groans, and psychiatric overtones).
• A chloride/phosphate ratio (> 33) suggests a PTH or PTHrP-mediated cause of hypercalcemia.
• 1,25-OH Vitamin D is the biologically active form of Vitamin D and can lead to hypercalcemia, but don’t forget to look at its precursor, 25-OH Vitamin D.
o If both are elevated, this suggests excessive Vitamin D intake.
o If just 25-OH Vitamin D is elevated, then search for an underlying granulomatous process.**Please note that there is an error in the actual PDF of the show notes.
The show notes read “If just 1,25-OH Vitamin D is elevated, then search for an underlying granulomatous process.”
The above sentence should read “If just 25-OH Vitamin D is elevated, then search for an underlying granulomatous process.
Clinical Reasoning Pearl
In certain scenarios, a “normal” value may be abnormal.
For example In patients with hypercalcemia, the parathyroid gland should completely suppress PTH production.If the PTH returns in the normal range, the problem must lie with the parathyroid gland