In addition to the resource linked below, please see
- Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome
Redefining an Illness (2015) Institute Of Medicine - Beyond Myalgic Encephalomyelitis/Chronic Fatigue Syndrome
Redefining an Illness: Report Guide For Clinicians Institute Of Medicine
In this post I link to and excerpt from Myalgic Encephalomyelitis/Chronic Fatigue Syndrome: Essentials of Diagnosis and Management, Mayo Clin Proc. 2021 Nov;96(11):2861-2878.
See also the above article’s supplemental tables PDF:
- SUPPLEMENTAL TABLE 1.
Potentially Abnormal Physical Examination Findings in ME/CFSa, pp 1 + 2 - SUPPLEMENTAL TABLE 2:
Tests to Be Considered Depending on Presentation, pp 3,4,5 - SUPPLEMENTAL TABLE 3.
Conditions Which Commonly Co-exist with ME/CFSa, pp 6 + 7
And here are the references from the supplemental tables PDF:
References
1. [This is a broken link*] Bateman L. “Simple way to assess orthostatic intolerance.” Bateman Horne Center. [
Published September 2016. http://batemanhornecenter.org/assess-orthostaticintolerance/ Accessed December 26, 2020.
*I have included additional links that cover the same subject.
-
-
- Passive standing tests for the office diagnosis of postural tachycardia syndrome: New methodological considerations. [PubMed Abstract] [Full-Text HTML] [Full-Text PDF]. Published online: 25 Aug 2018
- Orthostatic intolerance as a potential contributor to prolonged fatigue and inconsistent performance in elite swimmers [Full-Text]. BMC Sports Sci Med Rehabil. 2022; 14: 139.Published online 2022 Jul 23. doi: 10.1186/s13102-022-00529-8
- 10-Minute NASA Lean Test (a standardized passive stand test) for the diagnosis of orthostatic intolerance [Full-Text PDF] from the Bateman Horne Center (accessed 8-12-2022).
-
2. US ME/CFS Clinician Coalition. Testing recommendations for suspected ME/CFS.
Published February 20, 2021. https://mecfscliniciancoalition.org/mecfs-cliniciancoalition-testing-recs-v1 Accessed March 3, 2021.
3. US ME/CFS Clinician Coalition. Diagnosing and treating myalgic
encephalomyelitis/chronic fatigue syndrome (ME/CFS). Published July 2020.
https://mecfscliniciancoalition.org/mecfs-clinician-coalition-dx-tx-handout-v2
Accessed January 20, 2021. Also available in multiple languages on the US ME/CFS
Clinician Coalition website – https://mecfscliniciancoalition.org/ Accessed on January
20, 2021
4. US Institute of Medicine. Beyond myalgic encephalomyelitis/chronic fatigue
syndrome: redefining an Illness. Report guide for clinicians. The National Academies
Press. February 2015.
https://www.nap.edu/resource/19012/MECFScliniciansguide.pdf Accessed December
26, 2020.
All that follows is from the above resource.
Abstract
Despite myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) affecting millions of people worldwide, many clinicians lack the knowledge to appropriately diagnose or manage ME/CFS. Unfortunately, clinical guidance has been scarce, obsolete, or potentially harmful. Consequently, up to 91% of patients in the United States remain undiagnosed, and those diagnosed often receive inappropriate treatment. These problems are of increasing importance because after acute COVID-19, a significant percentage of people remain ill for many months with an illness similar to ME/CFS. In 2015, the US National Academy of Medicine published new evidence-based clinical diagnostic criteria that have been adopted by the US Centers for Disease Control and Prevention. Furthermore, the United States and other governments as well as major health care organizations have recently withdrawn graded exercise and cognitive-behavioral therapy as the treatment of choice for patients with ME/CFS. Recently, 21 clinicians specializing in ME/CFS convened to discuss best clinical practices for adults affected by ME/CFS. This article summarizes their top recommendations for generalist and specialist health care providers based on recent scientific progress and decades of clinical experience. There are many steps that clinicians can take to improve the health, function, and quality of life of those with ME/CFS, including those in whom ME/CFS develops after COVID-19. Patients with a lingering illness that follows acute COVID-19 who do not fully meet criteria for ME/CFS may also benefit from these approaches.Abbreviations and Acronyms:
CBT (cognitive behavioral therapy), GET (graded exercise therapy), ME/CFS (myalgic encephalomyelitis/chronic fatigue syndrome), NAM (National Academy of Medicine), PEM (post-exertional malaise)
In 2015, the US National Academy of Medicine (NAM, previously the Institute of Medicine) created new ME/CFS clinical diagnostic criteria that required the hallmark symptom of post-exertional malaise (PEM).1 The US Centers for Disease Control and Prevention have adopted these new criteria, have removed recommendations for CBT and GET, and have begun to incorporate the best clinical practices of ME/CFS experts. These steps will help improve the speed and accuracy of diagnosis and the quality of clinical care.
A study of patients ill 6 months after mild or moderate acute COVID-19 found that about half met criteria for ME/CFS.14
One review suggested that the number of cases of ME/CFS could double as a result of the pandemic.6 Like ME/CFS patients, those with post-COVID conditions have recounted being dismissed by health care professionals.15
This article provides essential information about how to diagnose and care for adults with ME/CFS and echoes other recent ME/CFS guidance.16, 17, 18 Accurately and expeditiously diagnosing ME/CFS is important. There are many steps a clinician can take to improve the health, function, and quality of life of these patients. Even if they do not go on to develop ME/CFS, some patients with post-COVID conditions may also benefit from approaches such as pacing.
Epidemiology
Myalgic encephalomyelitis/chronic fatigue syndrome affects between 836,000 and 2.5 million Americans of all ages, ethnicities, genders, and socioeconomic backgrounds.1
Mental health after the onset of ME/CFS is similar to that in other medical conditions and better than that seen in depression.24,25 The prevalence of depression and anxiety in ME/CFS is similar to that in other disabling, chronic illnesses.26,27
Impact and Prognosis of ME/CFS
Myalgic encephalomyelitis/chronic fatigue syndrome substantially impairs occupational, educational, social, and personal activities. The degree of impairment can exceed that of rheumatoid arthritis, multiple sclerosis, depression, heart disease, cancer, and lung disease.24,28,29 There is a wide spectrum of severity30 ranging from mild to very severe:
- Mild: mobile and self-caring; may continue working but will have reduced other activities
- Moderate: reduced mobility, restricted in instrumental activities of daily living, needs frequent periods of rest; usually not working
- Severe: mostly housebound; limited to minimal activities of daily living (eg, face washing, showering); severe cognitive difficulties; may be wheelchair dependent
- Very severe: mostly bedridden; unable to independently carry out most activities of daily living; often experience extreme sensitivity to light, sound, and other sensory input
Up to 75% are unable to work, and an estimated 25% are consistently housebound or bedbound.31,32 The level of severity can fluctuate, with 61% reporting being bedbound on their worst days.33
Although it is known that patients can be ill for years or even decades, no definitive study of prognosis exists. Studies are limited by small sample sizes, high dropout rates, short follow-up times, inclusion of patients with other conditions, and inappropriate definitions of recovery.34,35 A systematic review concluded that the chance of full recovery is only 5%.36 One ME/CFS-focused clinical practice estimated that 50% of its patients were still ill after 2 decades whereas a second estimated 93% (oral communication, US ME/CFS Clinician Coalition, March 2019).New Diagnostic Criteria
In 2015, the NAM published updated criteria. The new criteria require substantial impairment in function accompanied by fatigue, PEM, unrefreshing sleep, and either cognitive impairment or orthostatic intolerance (Figure). Symptoms should be of at least moderate intensity and present at least 50% of the time during a 6-month period. Other important factors include perionset infection, widespread pain, and impaired natural killer cell activity. Additional symptoms include influenza-like symptoms (eg, sore throat, tender lymph nodes); hypersensitivity to external stimuli (eg, food, smells, light, sound, touch, chemicals); susceptibility to infections; visual disturbances; gastrointestinal or genitourinary symptoms; respiratory issues, such as air hunger; and thermoregulatory issues.
The hallmark symptom of PEM is an exacerbation of some or all of a patient’s symptoms and a further reduction in functioning after physical, cognitive, orthostatic, emotional, or sensory challenges that were previously tolerated.
Notably, although postexercise fatigue and musculoskeletal pain are common in healthy people and other medical conditions (eg, osteoarthritis), the postexertional worsening of function and the constellation of symptoms (such as sleep, memory, concentration, influenza-like feelings [eg, sore throat], and mood) seen in ME/CFS are distinctive.
Etiology and Pathophysiology
While the exact etiology of ME/CFS is uncertain, studies show neurologic, immunologic, autonomic, and energy metabolism impairments.1 Key findings are highlighted here and described more fully elsewhere.1,44,45 Post-exertional Malaise and Energy Metabolism Impairment In both healthy and sick people, physical exercise improves fatigue, sleep, pain, cognition, and mood.46, 47, 48, 49 In contrast, patients with ME/CFS experience PEM, a distinctive exacerbation of the patient’s set of symptoms and a further reduction in functioning after previously tolerated physical, cognitive, orthostatic, emotional, or sensory stressors. Multiple studies using both patient-reported and physiologic outcome measures have confirmed these accounts.1,50, 51, 52
In the past, some physicians and scientists speculated that these exertional limitations were due to physical deconditioning or an irrational fear of activity.53 While chronically inactive people are likely to be deconditioned, deconditioning does not explain the symptoms of ME/CFS. Instead, evidence suggests that problems generating and using the main energy molecule, adenosine triphosphate (ATP), may be a fundamental driver of ME/CFS.54
Unrefreshing Sleep Patients experience various sleep disturbances, such as problems in falling or staying asleep. However, even when these problems are treated, most patients remain tired or sick on awakening. Reduced heart rate variability, controlled by the autonomic nervous system, is linked to unrefreshing sleep in ME/CFS and other conditions.73 Furthermore, studies have reported that nocturnal parasympathetic activity is decreased relative to sympathetic activity in ME/CFS, the inverse of what should be occurring during rest.74, 75, 76
Cognitive Impairment and Neurologic Abnormalities Decreased information processing speed is the most commonly found cognitive deficit in ME/CFS.1 Other abnormalities include decreased reaction time, working memory, and attention.77 These deficits are not due to poor effort, insomnia, or mood disorders.78,79 Defects become particularly prominent when patients face deadlines, unrelenting demands, and multiple simultaneous tasks.80 Motor speed, verbal abilities, and global reasoning remain intact. Brain studies have found brain inflammation and reductions in white matter and possibly in gray matter. Neuroinflammation is correlated with cognitive impairment and impaired connectivity across various regions of the brain.1,44
Objective physiologic abnormalities include the following:
- Abnormal heart rate and blood pressure changes after passive standing and tilt table tests81,82
- A 25% drop in cerebral blood flow on standing or sitting up83,84
- Decreases in stroke volume index and cardiac index that are not correlated with activity levels, contradicting theories that deconditioning explains ME/CFS85
- Orthostatic hypocapnia1,83 and a decrease in blood volume,86,87 which can further aggravate symptoms caused by abnormalities in the autonomic nervous system88
Gastrointestinal, urinary, thermoregulatory, and visual issues have also been reported but have not been extensively studied.1
Impaired Immune Function
On average, the natural killer cell activity of patients is lower than that of healthy controls.89, 90, 91 It is unknown whether this finding is a cause, consequence, or epiphenomenon of ME/CFS. Although patients with ME/CFS do not present with symptomatic, opportunistic infections (eg, cryptosporidiosis, tuberculosis), some do experience recurrent herpes infections.17,33 Some are susceptible to colds and may take longer to recover from infections, whereas others experience less frequent common infections (oral communication, US ME/CFS Clinician Coalition, May 2021).33 A quarter may have decreased immunoglobulins92 or have difficulty in controlling Epstein-Barr virus infections.93 Studies have also reported abnormal changes in T cells and cytokines.45
Infection Myalgic encephalomyelitis/chronic fatigue syndrome often follows an infectious illness,1,23 but the specific microorganism is often not identified because the illness initially appeared to be self-limited. Other times, ME/CFS follows a well-documented infectious illness, such as Epstein-Barr virus infectious mononucleosis or Giardia-caused diarrhea.1 In many patients with ME/CFS, reactivation of various latent infections (such as Epstein-Barr virus infection) has also been observed,94 but it is unclear whether they cause symptoms or just reflect a suppressed or “distracted” immune system.95 Alternatively, the chronicity of ME/CFS could be the result of an infection-triggered autoimmune response.96
Diagnostic Approach
The purpose of initial evaluations is to determine whether alternative conditions may account for all of the patient’s symptoms, to confirm ME/CFS through recognition of characteristic symptoms and signs, and to identify comorbid conditions. Because there are no definitive diagnostic tests, diagnosis relies on medical history and physical examination and may require multiple visits. Tests and referrals to specialists are used primarily to identify alternative diagnoses and comorbidities.
Typical Presentation: Important Elements of the History
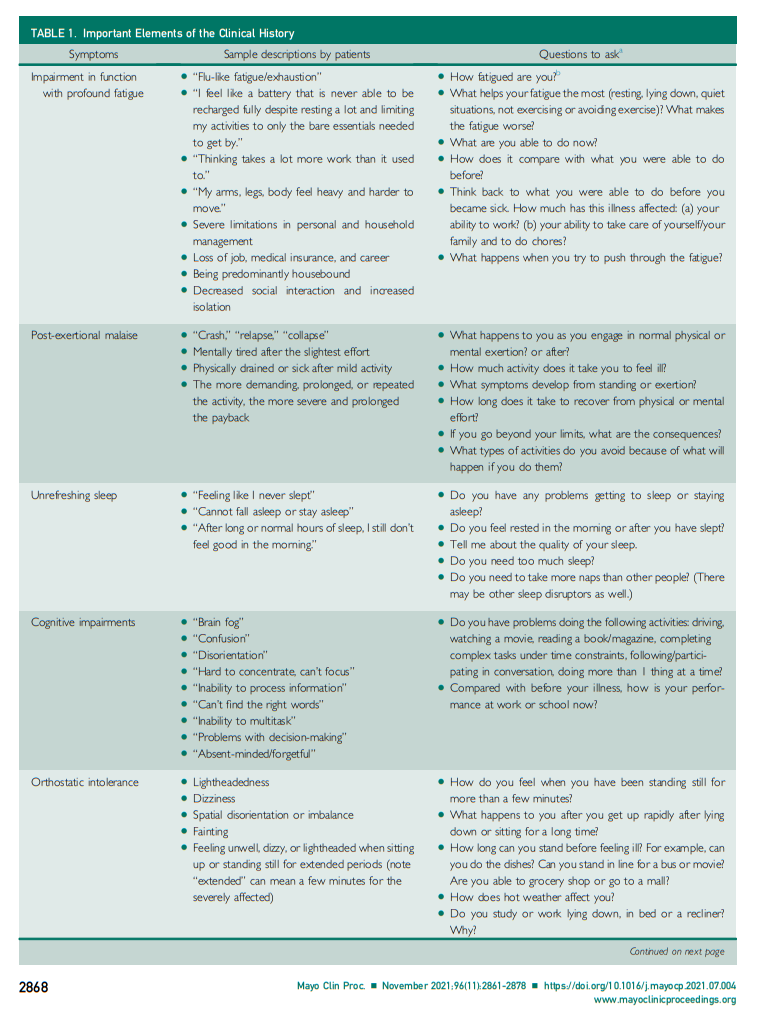
Patients typically experience a proven or nonspecific infection but fail to recover as expected and continue to be ill weeks to months later. Some patients may identify a noninfectious trigger (eg, surgery, pregnancy, vaccination) or no precipitant at all. Chronologic patterns can vary. In some patients, all of the ME/CFS symptoms develop within hours or days of the instigating event, whereas others report symptoms appearing more gradually over weeks and months. Patients often describe a waxing and waning pattern or sometimes remission to normal health followed by relapse.Patients may initially complain of persistent influenza-like symptoms, sleep disturbances, problems in thinking, profound fatigue, problems in being upright, and difficulty in keeping up with normal activities. They may struggle with school, work, family responsibilities, exercise, socializing, or personal care. They may complain of pain and hypersensitivities to light, sound, fragrances, food, and medications. Patients may be susceptible to mold or other environmental toxins. They may experience other symptoms but not link them to their illness or have difficulty describing them. Consequently, it is important for clinicians to ask explicitly about the symptoms composing the criteria for ME/CFS. Examples of questions to ask are listed in Table 1. Family members may need to respond for the most severely ill.
The key symptom of PEM is often not mentioned spontaneously as patients may not be familiar with the concept. The nature and severity of PEM symptoms, the degree of reduction in function, and PEM’s time course can vary from episode to episode and with the type of activity. If the patient is unable to clearly answer the PEM questions suggested in Table 1, ask the patient to keep a journal for 1 or 2 weeks detailing activities and symptoms (type, intensity, frequency, duration). The patient may be in a constant state of PEM, making it difficult to recognize the impact of overexertion. During the next visit, clinicians should review this journal with the patient to identify the distinctive features of PEM: odd symptoms that would not normally follow exertion (eg, sore throat, problems in thinking), intensity or duration of symptoms out of proportion to preceding activities (eg, having to lie down for an hour after a few hours of sedentary work), a further reduction of function after activity, and typically delayed onset of symptoms (eg, a few hours or a day later).98,99
Orthostatic intolerance commonly is manifested as lightheadedness, palpitations, or syncope. However, patients with ME/CFS often experience subtler symptoms, such as feeling sick, nauseous, tired, or confused during periods of sitting or standing still.100 Inquiring about symptoms during aggravating (eg, long lines, hot weather) and alleviating situations (eg, lying, sitting down) is helpful. Patients may have been diagnosed with anxiety as some symptoms (eg, lightheadedness, a “racing heart”) are shared by both conditions. Accurate identification of orthostatic intolerance avoids misdiagnosis with a psychiatric disorder and ensures its appropriate management, which is different from that of anxiety.18*,100**
*Rowe P.C. Underhill R.A. Friedman K.J. et al.
Myalgic encephalomyelitis/chronic fatigue syndrome diagnosis and management in young people: a primer.
Front Pediatr. 2017; 5: 121
Crossref PubMed Scopus (62) Google Scholar
**Rowe P.
General information brochure on orthostatic intolerance and its treatment. March 2014.
https://www.dysautonomiainternational.org/pdf/RoweOIsummary.pdf
Date accessed: December 26, 2020
Google Scholar
Some patients are so affected by cognitive dysfunction that they cannot converse, read a book, follow directions, or remember what was just said. Other patients function reasonably well for brief periods but suffer from cognitive fatigue or reduced or slowed abilities under time or other pressures. Many patients stop or restrict driving because of these issues.
The most severely ill patients are bedbound and unlikely to be seen in the clinician’s office but may be seen in emergency departments and hospitals during a crisis.101 Whether in the hospital or at home, the very severely ill require individualized care that accounts for their severe energy limitations and sensory sensitivities. The recent expansion of telemedicine may facilitate the provision of care for all ME/CFS patients. Management of the severely ill is further described by Kingdon et al102 and Speight.103
Physical Examination
Abnormal physical findings may be absent, particularly if the patient has rested extensively before the office visit. Some nonspecific abnormal physical examination findings may exist and may worsen during the course of an office visit (Supplemental Table 1, available online at http://www.mayoclinicproceedings.org). Whereas the absence of these signs does not exclude ME/CFS, their presence may support an ME/CFS diagnosis.The physical examination may help identify alternative diagnoses and comorbidities. The neurologic examination, in particular, may eliminate neurologic disorders. Abnormal physical findings beyond those associated with ME/CFS should be followed up as potential indications of other conditions (Supplemental Table 1).
Diagnostic TestingThere is no validated diagnostic test. Basic tests recommended for all patients (Table 2) or tests for a particular presentation (Supplemental Table 2, available online at http://www.mayoclinicproceedings.org) may be used to identify alternative conditions and comorbidities.104
Diagnostic Testing
There is no validated diagnostic test. Basic tests recommended for all patients (Table 2) or tests for a particular presentation (Supplemental Table 2, available online at http://www.mayoclinicproceedings.org) may be used to identify alternative conditions and comorbidities.104*
*US ME/CFS Clinician Coalition Testing recommendations for suspected ME/CFS. February 20, 2021. [This resource should be carefully reviewed by all clinicians. It is outstanding.]
https://mecfscliniciancoalition.org/mecfs-clinician-coalition-testing-recs-v1
Date accessed: March 3, 2021
Google Scholar
Some tests can be used to characterize aspects of ME/CFS. The passive standing or tilt table tests can objectively confirm orthostatic intolerance.105* A 4-point salivary cortisol test can help identify the abnormal diurnal cortisol patterns seen in ME/CFS (oral communication, US ME/CFS Clinician Coalition, March 2019).
*Bateman L.
“Simple way to assess orthostatic intolerance.” Bateman Horne Center. September 2016.
http://batemanhornecenter.org/assess-orthostatic-intolerance/
Date accessed: December 26, 2020 [Both clinicians and patients will benefit from carefully reviewing the resources on this page.]
Google Scholar
Testing can also guide treatment decisions and objectively document disability. For instance, ME/CFS experts may use microbial panels and natural killer cell activity,1 a measure of immune functioning, to help guide treatment decisions. Neuropsychological testing can demonstrate cognitive impairment and repeated cardiopulmonary exercise testing an inability to repeat or to sustain physical activities. However, these tests involve a challenge that may induce severe or long-lasting PEM. This risk may be warranted for disability evaluations,106* but they are not recommended as a diagnostic aid in all patients.
*Podell R. Dimmock M.E. Comerford B.B.
Documenting disability in myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS).
Work. 2020; 66: 339-352
Crossref [Link is to the full text] PubMed Scopus (2) Google Scholar
Alternative Diagnoses
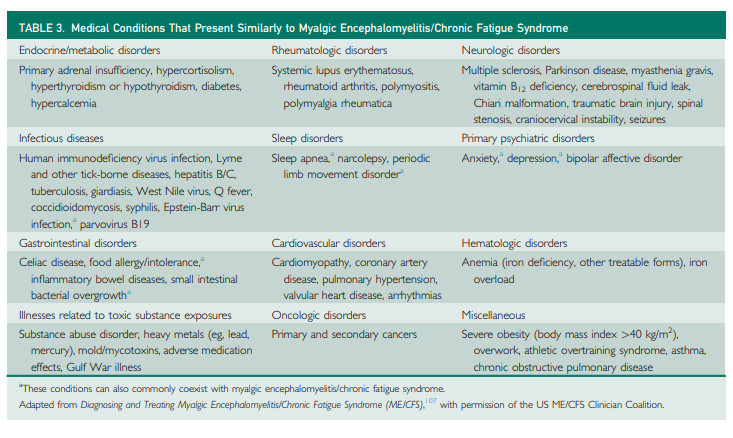
Symptoms of ME/CFS can overlap with those of a number of medical and psychiatric conditions (Table 3).107 At the same time, patients can have both ME/CFS and other diseases. History, physical examination, screening instruments, and diagnostic tests can help distinguish other conditions from ME/CFS. For example, fatigue and a reduction in activities can be seen in both ME/CFS and depression or anxiety; but PEM and orthostatic intolerance are not characteristic of mood disorders, whereas feelings of worthlessness are typically absent in ME/CFS.18,26 In general, PEM is a distinctive feature that can help differentiate ME/CFS from other diseases. Therapeutic trials may also help; if treatment for the alternative diagnosis completely eliminates a patient’s symptoms, ME/CFS is not the correct diagnosis.
Alternative Diagnoses
Symptoms of ME/CFS can overlap with those of a number of medical and psychiatric conditions (Table 3).107
At the same time, patients can have both ME/CFS and other diseases. History, physical examination, screening instruments, and diagnostic tests can help distinguish other conditions from ME/CFS. For example, fatigue and a reduction in activities can be seen in both ME/CFS and depression or anxiety; but PEM and orthostatic intolerance are not characteristic of mood disorders, whereas feelings of worthlessness are typically absent in ME/CFS.18,26 In general, PEM is a distinctive feature that can help differentiate ME/CFS from other diseases. Therapeutic trials may also help; if treatment for the alternative diagnosis completely eliminates a patient’s symptoms, ME/CFS is not the correct diagnosis.
The NAM criteria require that symptoms exist for 6 months because acute medical conditions or lifestyle issues should resolve within that time. During these 6 months, the provider should observe patients closely to detect other causes for their symptoms while also beginning treatment as discussed later.
Diagnosis of Comorbidities
Myalgic encephalomyelitis/chronic fatigue
syndrome is often associated with various
comorbidities that can contribute substantially to the patient’s symptom burden
(Supplemental Table 3, available online at
http://www.mayoclinicproceedings.org).107MANAGEMENT APPROACH
Treat the Symptoms of ME/CFS
Although there are no approved treatments
specific to ME/CFS, clinicians can reduce the
severity of symptoms with standard pharmacologic and nonpharmacologic treatments.123Nonpharmacological approaches
(Table 4) for orthostatic intolerance include
salt and fluid loading and compression
stockings, whereas memory aids (notebooks,
calendars) may help with cognitive issues.
Patients may also be helped by ear plugs,
eye masks, and sunglasses to minimize light
and noise intrusion; sleep hygiene measures
(tailored as needed for patients who are bedbound or have orthostatic intolerance); and
avoidance of certain foods to decrease
gastrointestinal disturbances.17,18,123Experts in ME/CFS have had success
with a range of pharmacologic therapies
(Table 4).123 Sleep may be improved with
medications, such as trazodone, clonazepam,
tricyclic antidepressants, and suvorexant.
Methylphenidate, modafinil, or dextroamphetamine can occasionally help with cognitive issues, but there is a risk of addiction
with methylphenidate and dextroamphetamine. Patients with ME/CFS and clinicians report improvement from therapies such as
fludrocortisone and fluid expansion.18,115,123
On occasion, patients may require intravenous
administration of fluids for severe orthostatic
intolerance episodes. Medications such as
gabapentin, pregabalin, low-dose naltrexone,
and duloxetine may be used to treat pain.Medications should be initiated at lower
dosages and slowly titrated up to avoid
triggering drug sensitivities common in
ME/CFS. To reduce polypharmacy, medications that treat more than 1 symptom should
be favored. Clinicians should also be aware
of sensitivities to anesthesia and medication
ingredients considered to be inactive
(eg, fillers, vehicles, preservatives).Some disease experts have selectively
used antivirals and immune modulators offlabel in some patients and have observed
favorable responses (oral communication,
US ME/CFS Clinician Coalition, March
2018 to March 2021). A specialty consultation may be helpful in developing a treatment plan and in managing those aspects
of the disease with which the referring
physician is unfamiliar.Treat Comorbidities
start here.