In this post I link to and excerpt from the outstanding medical education website, ddxof.com by Dr. Tom Faidal*, [This link is to his home website], Assistant Professor of Emergency Medicine [This link is to his faculty website page].
*Dr. Faidal has a number of great websites and resources that you can explore [the links above].
And here is the header of the ddxof.com home page:
ddxof: is a compilation of cases based on real patients, each inspiring an algorithm for the evaluation and management of their chief complaint or diagnosis.
* You definitely want to download Dr. Faidal’s excellent app.
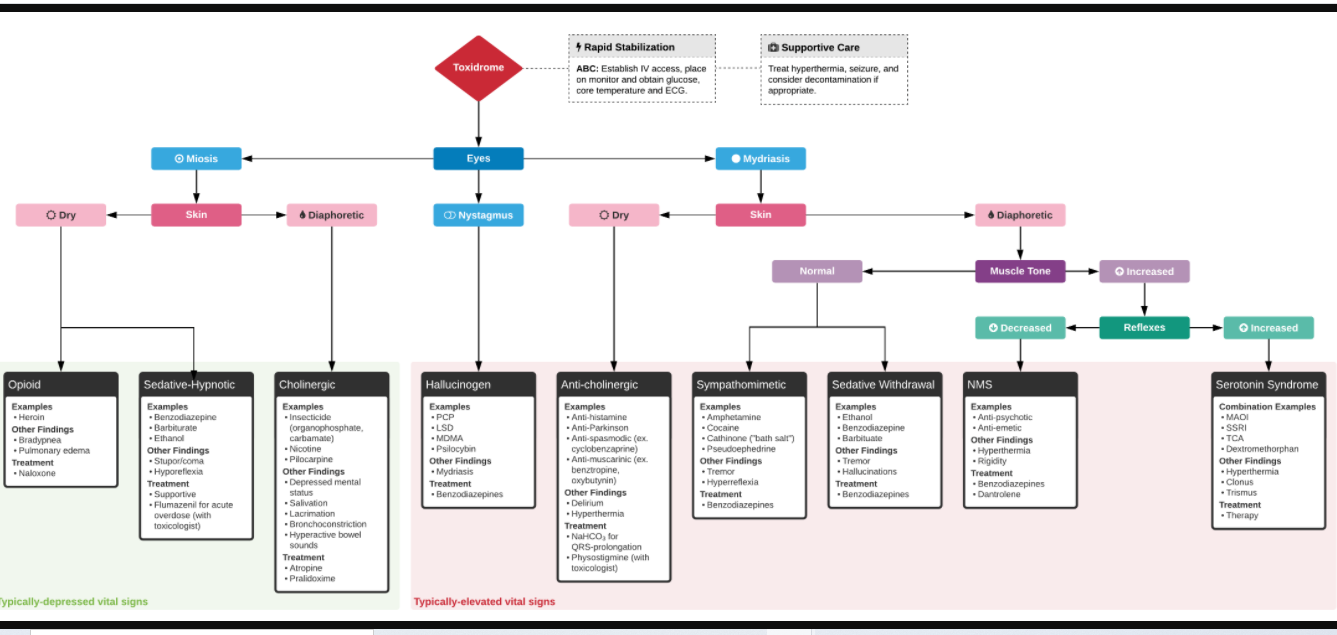
So today, I link to and excerpt from Toxidromes posted in Toxicology on September 21, 2020 by Dr. Faidal.
Here are excerpts:
Case 1:
A 20 year-old male with a history of polysubstance use, depression and seasonal allergies presents via ambulance for altered mental status. According to prehospital report, EMS were contacted by the patient’s roommate who noted that he had been acting strangely after being alone in his room for several hours. Vital signs are notable for fever (T 103.2°F) and tachycardia. The patient was confused, unable to follow commands – pupils were dilated.
The initial impression was concerning for sympathomimetic toxicity, the patient was treated with cooled intravenous fluids and required pharmacologic sedation and physical restraints to obtain blood samples. ECG, initial laboratory tests and urine toxicology screen were unremarkable. A non-contrast CT head was normal.
The patient remained altered and a repeat examination was performed which revealed multiple, opened blister packs of diphenhydramine and dry, flushed skin.
Anti-cholinergic toxicity was presumed, likely exacerbated by the administration of butyrophenones for sedation. He was treated with benzodiazepines, additional evaporative cooling measures and was admitted to the intensive care unit.
Case 2:
A32 year-old female with a history of depression was brought to the emergency department by family members who were concerned about bizarre behavior and muscle stiffness. They note that the patient was recently started on a new antidepressant though they are unsure of the name. They describe occasional alcohol consumption but no illicit drug use.
In the emergency department, vital signs were notable for fever and hypertension. Examination demonstrated increased muscle tone and sustained clonus in bilateral lower extremities.
The patient’s presentation was concerning for serotonin syndrome, she was treated with benzodiazepines and intravenous fluids with gradual improvement in mental status and hypertonicity. Upon awakening, she reported doubling her medication dose recently due to persistent feelings of hopelessness as well as increased wine consumption.
Here is a direct link to the chart below that is much clearer than my copy.
And here are excerpts from Dr. Faidal’s article that follows his algorithm:
Diagnostic Tests
ALL PATIENTS MOST PATIENTS CRITICAL PATIENTS POC glucose Core temperature
ECG
Urine hCG
BMP UA
Acetaminophen
Salicylate
Ethanol
LFT Lipase
Serum osmolarity
Ionized calcium
Magnesium
GI Decontamination – See article for details including use of activated charcoal and whole bowel irrigation.
Serum alkalinization – See article for details.
Intralipid emulsion
May be useful for local anesthetic toxicity, b-blocker, and calcium channel blocker overdose.
Electrocardiographic Toxidromes
QT PROLONGATION QRS PROLONGATION Anti-emetic Diphenhydramine Anti-psychotic Cocaine Anti-microbials (fluoroquinolone, macrolide) Diltiazem, verapamil Anti-depressant (TCA, SSRI) Propranolol Anti-arrhythmic Amantadine Carbamazepine Gap-producing Toxidromes
Osmolar Gap
- Toxic alcohol
- Ethanol
- Methanol
- Ethylene glycol
- Isopropyl alcohol
- Drug stabilizing agents
- Mannitol
- Propylene glycol
- Glycerol
Anion Gap
- Salicylate
- Iron
- Isoniazid
- Methanol
- Ethylene glycol
- Cyanide