Note to myself: the article reviewed in this post is not, for me, worth reviewing again. I leave the post in to avoid breaking links.
Useful resources when treating rhinitis, sinusitis, or rhinosinusitis are:
- Nonallergic Rhinitis – Excerpts and Resources
Posted on December 14, 2018 by Tom Wade MD- This post discusses and has resources on the use of nasal steroids, nasal antihistamines, and nasal anticholinergics.
- Medical Outcomes Study Questionnaire Short Form 36
Health Survey (SF-36) [Link is to the PDF] - A Great Resource On Sinus Disease-#239 Sinusitis: It’s Not That Tricky-From Dr Jardine And The Curbsiders
Posted on October 28, 2020 - Adult Rhinoconjunctivitis Quality of Life Questionnaire
- Paediatric Rhinoconjunctivitis Quality of Life Questionnaire
In this post I link to and excerpt from Rhinitis Quality of Life in Clinical Practice
[Link is to the PDF] ELIZABETH F. JUNIPER MCSP, MSC.
Here are excerpts:
Is there a place for health-related quality of life in clinical practice?
There is a range of efficacious medications now available
for the treatment of rhinitis as well as clear guidelines for
their use. However, low rates of patient compliance can
pose a major challenge to effective rhinitis management. An
important contributor to poor compliance may be a
discrepancy between the goals of the clinician and those of
the patient. Clinicians tend to focus on nasal impairments by
measuring outcomes like nasal symptom severity, nasal
patency and inflammatory cytology. In contrast, patients,
although bothered by their symptoms, are usually more
concerned with their ability to function normally in their
day-to-day lives. Improved clinician awareness of patients’
rhinitis-related quality of life goals and a willingness to
address them may enhance patients’ willingness to take
medications and thus improve both their health-related
quality of life (HRQL) and the clinical status of the nose.
Therefore, there is a need for quick, valid, easy-to-use, self-administered and clinic friendly quality of life questionnaires. The responses to these questionnaires can be used during the consultation to identify patients’ greatest problems, ascertain how troublesome they are and ensure that they are addressed in the treatment plan. Questionnaires can also be used to monitor patient progress over time.What is health-related quality of life?
The quality of a person’s life may be considered in terms of
its richness, completeness and contentedness. A number of
factors contribute to this sense of well-being and include
good health, a secure social and occupational environment,
financial security, spirituality, self-confidence and strong,
supportive family relationships. Each factor may be a
determinant of a person’s quality of life and may be closely
interrelated with each of the others. For instance, a patient
will often be able to deal with an illness better if he/she has
good family support, a strong faith and the financial ability
to acquire nourishing food, shelter and treatment.
Health-related quality of life can be considered as that part
of a person’s overall quality of life that is determined
primarily by health status and which can be influenced by
clinical interventions. The definition by Schipper and
colleagues is both simple and focussed: “the functional
effects of an illness and its consequent therapy upon a
patient, as perceived by the patient”(1). The final phrase is
important because it emphasises that these are the
impairments that patients themselves consider important.Why is quality of life important in rhinitis?
There are three reasons for treating patients: to prevent
mortality; to reduce the probability of future morbidity; and
to improve patient well-being (quality of life) (2). Rhinitis
rarely causes mortality and so the primary goals of
treatment are usually to prevent permanent damage to the
nasal mucosa and improve quality of life. Most conventional
clinical outcomes measure the status of the nose and
usually include such things as severity of nasal symptoms,
rhinomanometry, acoustic rhinometry, nasal peak flow,
nasal hyper-reactivity and inflammatory cytology. In the
past, it was frequently assumed that these measures also
provided insight into patients’ well-being. Certainly,
patients with very severe persistent rhinitis tend to have a
worse quality of life than patients with milder intermittent
rhinitis, but quality of life does not correlate closely with
clinical status (3). Even the correlation between severity of
symptoms and the impact that they have on the patient is
only modest. Therefore the impact of rhinitis on a patient’s
quality of life cannot be inferred from the clinical indices, it
must be measured directly.What are the problems that bother patients?
Rhinitis may be a non-life threatening condition but it has an
enormous impact on patients’ ability to function normally in
day-to-day activities (physical, social, occupational and
emotional). This impact is often not recognised by clinicians
and there has been a tendency to dismiss the condition as
trivial as many cases resolve spontaneously at the end of a
pollen season or cessation of exposure to other allergens.
However, when symptomatic, patients often experience
worse impairment in quality of life than patients with more
persistent chronic conditions such as asthma (4,5).Can quality of life questionnaires help in clinical practice?
As I have already identified, patients are treated for three
reasons: to prevent mortality, to reduce the probability of
future morbidity and to improve patient well-being (quality
of life). I would like to propose that in the majority of cases,
quality of life should be the primary outcome of importance
for both the clinician and the patient. Rhinitis is non-life
threatening and rarely causes long-term permanent damage
to the nasal passages.However, clinicians treating rhinitis tend to focus on morbidity and they use the conventional clinical outcomes to assess the status of the nasal mucosa.
[But] Most patients seek help from their clinicians in order to feel better and to function better in their every day activities.
They want to be able to enjoy their sports, function well at
work, participate social activities with their friends and
family and cope easily with day-to-day activities of living.WHAT IS SHARED-DECISION MAKING?
Shared-decision making (10) is an approach to patient management in which the clinician and the patient decide
together on the patient’s management plan (Table 3). In rhinitis, the clinician brings to the encounter expertise in diagnosis, the goals of clinical rhinitis management and rhinitis treatment options.The patient brings to the encounter his/her own goals for improving rhinitis related quality of life, concerns about
medications and likes/dislikes of various forms of treatment regimens. Together, the clinician and patient negotiate a rhinitis
management plan that works towards both their goals and which, most .importantly, the patient is willing to follow.Quality of life questionnaires may have an important role by facilitating the identification of patients’ goals and concerns. After the patient has completed the questionnaire in the waiting room, a quick scan of the responses allows the clinician to focus on problems that are most troublesome and this quickly leads to the identification of the patient’s treatment goals.
How do i select the right questionnaire for the task?
TYPES OF QUESTIONNAIRES
Generic Health Profiles
There are two types of quality of life questionnaires, generic
and specific. Generic health profiles can be used in patients
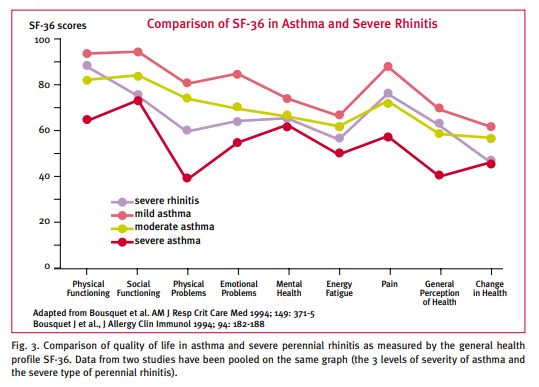
with all medical conditions. In adults, the most commonly
used and the best validated is the Medical Outcomes Survey
Short Form 36 (SF-36) [Link is to the PDF of SF-36](15) (Figure 3).