In this post, I link to and excerpt from the following resource on Oncologic Emergencies from:
- 11 Oncologic Emergencies You Need to Know
Nicole Cimino-Fiallos, MD, FAAEM | June 5, 2019
- Introduction
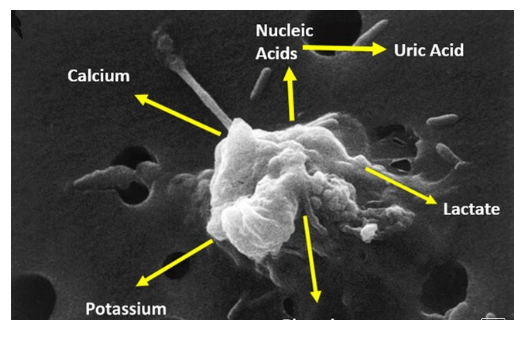
- Tumor Lysis Syndrome
- Hypercalcemia of Malignancy
- Neutropenic Fever
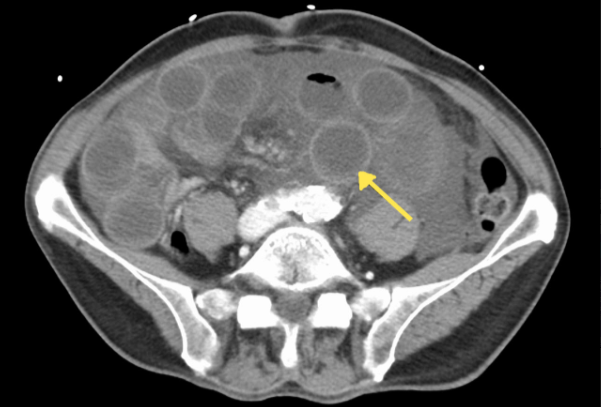
- Typhylitis (Neutropenic Enterocolitis)
- Hyperviscosity Syndrome
- Hyperviscosity Syndrome Clinical Presentation
Updated: Dec 11, 2019
Author: Thomas J Hemingway, MD, FACEP from emedicine.medscape.com- Hyperviscosity Syndrome Workup
Updated: Dec 11, 2019
Author: Thomas J Hemingway, MD, FACEP from emedicine.medscape.com- Superior Vena Cava Syndrome
- Epidural Spinal Cord Compression
Here are excerpts:
Adapted electron micrograph of a cell undergoing apoptosis from the National Cancer Institute / Susan Arnold.
Electrocardiogram (ECG) depicting combined hyperkalemia and hypocalcemia from Wikimedia Commons / Jer5150.
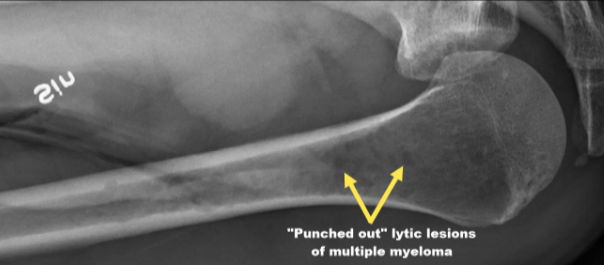
Image of a left humerus with lytic lesions associated with multiple myeloma from Wikimedia Commons / Mikael Häggström.
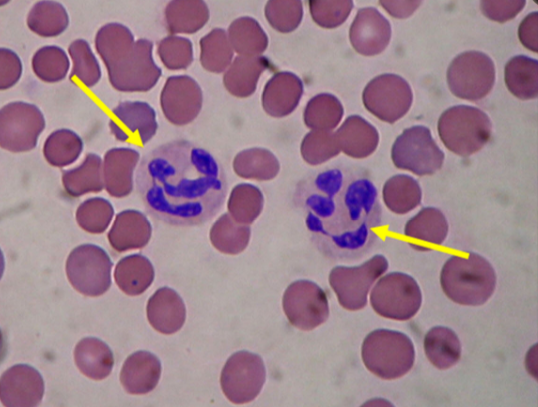
Image of neutrophils (arrows) in a peripheral blood smear from Wikimedia Commons.
Table from Villafuerte-Gutierrez P, Villalon L, Losa JE, Henriquez-Camacho C. Adv Hematol. 2014;2014:986938. [Open access.] PMID: 25525436, PMCID: PMC4265549
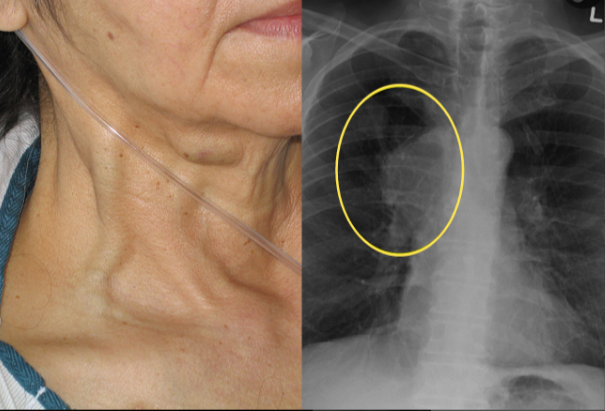
Image from Wikimedia Commons / James Heilman, MD.
Image of a plasmapheresis device from Wikimedia Commons.
Hyperviscosity Syndrome Clinical Presentation
Updated: Dec 11, 2019
Author: Thomas J Hemingway, MD, FACEP from emedicine.medscape.comThe clinical presentation of hyperviscosity syndrome consists principally of the triad of mucosal bleeding, visual changes, and neurologic symptoms. [3] Constitutional symptoms and cardiorespiratory symptoms also contribute to the clinical presentation.
The tendency to bleed is the most common manifestation of hyperviscosity syndrome. Patients may present with any of the following:
Visual changes range from blurred vision to vision loss. Neurologic manifestations are frequent and varied, and may include the following:
Other manifestations may include heart failure, shortness of breath, hypoxia, fatigue, and anorexia. In fact, the clinician should have a high index of suspicion for hyperviscosity syndrome in patients with unexplained coma/altered mental status or unexplained shortness of breath, especially in those with an underlying hematologic disorder.
Blood hyperviscosity plays a role in the pathogenesis of several cardiovascular diseases, including hypertension, atherosclerosis,and the metabolic syndrome. [8]
Physical findings are related to the major organ systems involved, as follows:
Bruises, epistaxis, or gum bleeding may be noted
Ophthalmic examination may reveal decreased visual acuity, dilated retinal veins, “sausage-linked” or “boxcar segmentation” of the retinal veins, or retinal hemorrhages [9]
Neurologic examination may reveal various abnormalities, including diminished mental status, confusion, ataxia, or nystagmus
Cardiopulmonary examination may reveal signs of congestive heart failure with volume overload (rales, lower extremity edema, elevated jugular venous pressure, and hypoxia)
Hyperviscosity Syndrome Workup
Updated: Dec 11, 2019
Author: Thomas J Hemingway, MD, FACEP from emedicine.medscape.comThe diagnosis of hyperviscosity syndrome (HVS) is confirmed by measurement of elevated serum viscosity in a patient with characteristic clinical manifestations of HVS. No exact diagnostic cut-off exists for serum viscosity, as different patients will have symptoms at different values. A clue to the need for measurement of serum viscosity may be that the laboratory has difficulty performing chemical tests, because hyperviscous blood can clog analyzers.
The normal reference range for serum viscosity is 1.4-1.8 Centipoises (1.0 being the viscosity of water). Symptoms usually are not seen before the viscosity reaches 4 Centipoises, and patients with HVS usually present with a serum viscosity greater than 5 Centipoises. Typically, the higher the viscosity, the worse the symptoms.
For further details of the workup of hyperviscosity syndrome please see the link to the article.
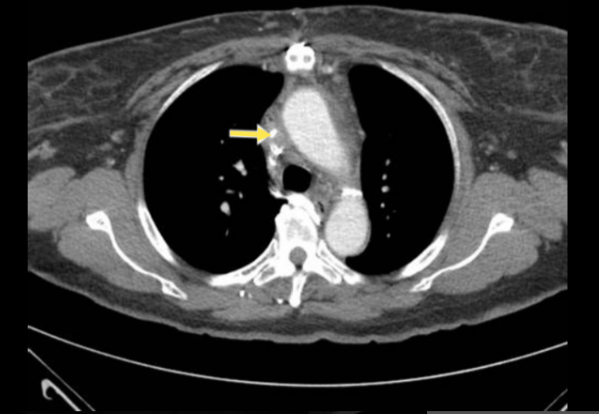
Chest CT scan with contrast showing narrowing of the SVC from Senthilvel E, Papadakis A, Jain V, Bruner J. Cases J. 2009;2:6463. [Open access.] PMID: 19829810, PMCID: PMC2740218.
Start here.