Resources:
Strep Pharyngitis BY DR SEAN FOX of Pediatric EM Morsels. PUBLISHED DECEMBER 3, 2010 · UPDATED NOVEMBER 21, 2013. The following are excerpts from the above post:
Background
– Pharyngitis is most commonly caused by viral infections.
– Bacterial play a much smaller; Group A Strep (GAS) is the leader of this small pack.
– GAS is primarily a disease of children (5-15yrs is the “sweet spot;” however, it does occur in younger and older.
– GAS is a self-limited disease!So why do we care?
– GAS can lead to complications, of which, it is Acute Rheumatic Fever (ARF) that we aim to prevent with treatment of GAS.
– During epidemics, ~3% of GAS left untreated may lead to ARF. With GAS occurring in isolated sporadic events, the incidence of ARF is much lower.
– Primary ARF is generally a disease of the young (oldest case report that I have found was a 38yr old, which is young by my standards).Secondary ARF can occur at any age; once you have had it, ARF recurs easily.
– ~60% of ARF will develop Rheumatic Heart Disease (which is why we care).Accurate diagnosis of GAS
– Unfortunately nothing is perfect. The physical findings overlap between GAS and Viral etiologies.– CENTOR CRITERIA
> 1) Tonsillar Exudates, 2) Tender cervical LAD, 3) Absence of cough, 4) Fever
> Each criteria = 1 point.
> Positive Predictive Value of 3 or 4 points = ~40% (~60% would have negative throat culture)
> Negative Predictive Value of a score of 0 = ~81%
> Works better to rule-out the condition rather than rule it in.– Throat Culture requires “vigorous swabbing on both tonsils and posterior pharynx.”
– RADT – a negative result does not rule-out the condition, so culture is needed to confirm results.
– Because of lower incidence of GAS and even lower risk of ARF in adults, no confirmatory test is recommended.My interpretation of what the AHA recommends
– Use Centor Criteria to determine whether your pre-test probability is low enough to avoid testing.
– If you have no access to RADT, then use clinical suspicion and high Centor scores to treat empirically. Alternatively, a throat culture can be sent and antibiotic therapy delayed (you have more than a week (~10 days) before ARF would develop).
– If you have access to RADT, use it. Treat if positive. Send culture if negative and delay antibiotic therapy until result returns (unless it is an adult, in which case do not send culture).– I would refrain from performing a test that I did not then act upon. Ask yourself whether you are going to ignore a negative RADT prior to doing it. If you are, then don’t do it. Although, I would prefer to ensure that I get an adequate sample and believe the test. That being said, we’ve all encountered that patient who made you break into a sweat to even get past his or her lips. In that case, if I don’t believe that I got an adequate sample, I won’t send the test and will either have the kid follow-up in another day or so to re-evaluate or treat empirically, depending on the H+P (and the phase of the moon).
Perianal Strep Infection BY DR SEAN FOX of Pediatric EM Morsels· PUBLISHED MAY 6, 2011 · UPDATED OCTOBER 15, 2015. The following is from the Perianal Strep Infection post:
Naturally, we are all accustomed to evaluating children for rashes. Most often I am simply attempting to define the lack of characteristics that are concerning for more significant medical conditions (petechiae, purpura, vesicles, bull, target lesions, urticaria, desquamation). Then I consider whether this is a presentation of typical childhood illness (Fifth’s Disease, molluscum contagiosum, pityriasis rosea, etc). Here is a condition that is often forgotten about that you can add to your list of typical childhood rashes… one that many times gets overlooked and called “diaper rash:” Perianal Strep.
- Usually occurs in children <10 years of age – particularly infants and pre-school aged kids.
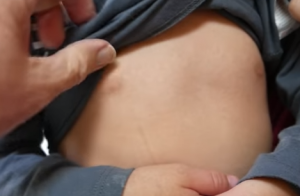
- Group A Streptococcus pyogenes (Yes the same that causes “Strep Throat”) can cause local skin infection in the perianal region (just as it can in skin folds – see Intertrigo).
- Presentation includes:
- Well-demarcated red area surrounding the anus (usually “Beefy-red” and usually extending 2cm around the anus) – sometimes with exudates
- Tenderness
- Painful defecations (leading to constipation due to toileting aversion)
- Itching
- Fissures
- Bloody streaks in stool
- Vulvovaginits
- Often misdiagnosed as:
- Pin-worm infection
- Candidiasis
- Diaper Dermatitis
- Simple anal fissures
- Sexual abuse
- You can diagnosis it as you would Strep Throat – with a Rapid Strep test and a Culture
- Treatment:
- Oral Penicillin VK or Clarithromycin or Augmentin for 7-10 days.
- The efficacy of topical therapies is questionable.
Group A Strep Infections and Associated Rhinitis – 2:52 YouTube Video from Dr. Larry Mellick’s YouTube Channel, Published on Oct 18, 2017. What follows are some excerpts from the video:
Dr. Mellick summs up the video by saying:
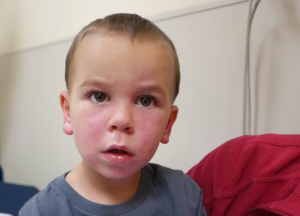
The teaching point of the video is that just because a child has a runny nose, doesn’t mean that they don’t have a strep throat. . . because younger kids will sometimes present [with a runny nose and they can still have a strep infection].
And reviewing the first two slides of Dr. Mellick’s video we are reminded that:
And that:
See also Strep Throat and Scarlet Fever – 2:11 YouTube Video from Dr. Larry Mellick’s YouTube Channel, Published on Dec 11, 2011:
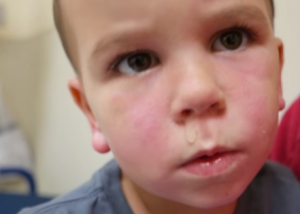
Prominent red lips as well as circumoral pallor are two physicial findings associated with Group A Streptococcal infections of the throat. The prominent red lips finding was recently described in the Pediatric Emergency Care Journal in 2009. Additionally, the Scarlet Fever rash in African American children is unique appearing in that the “scarlet” is missing and the fine papular rash of scarlet fever is actually more coarse in texture.