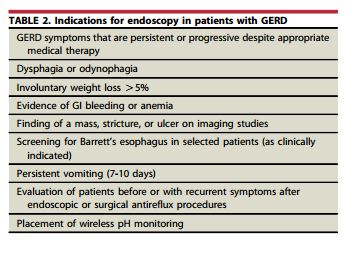
After reviewing the HHS report on Joan Rivers endoscopy, I wanted to review the indications for upper GI endoscopy in patients with symptoms of dyspepsia or reflux.
The American Society for Gastrointestinal Endoscopy (ASGE) recommends endoscopy for all patients over the age of 50 yrs who have dyspepsia or reflux symptoms even in the absence of other alarm symptoms.
The British National Institute for Health and Care Excellence (NICE) Resource (5) recommends considering upper GI endoscopy in patients over the age of 55 years with treatment resistant dyspepsia to evaluate for esophageal and stomach cancer. See the resource for other detailed recommendations.
********************************************************************************
What follows are excerpts from this guideline:
The role of endoscopy in the management of GERD [PubMed Abstract] [Full Text HTML] [Full Text PDF] from the American Society of Gastrointestinal Endoscopy. GASTROINTESTINAL ENDOSCOPY Volume 81, No. 6 : 2015.
GERD is a condition that develops when reflux of stomach
contents causes troublesome symptoms (eg, heartburn
and regurgitation) or adverse events (eg, erosive esophagitis).3-5
In a recent systematic review, the prevalence of
GERD in the United States was estimated to be 18% to
28%, when GERD was defined as at least weekly heartburn
and/or acid regurgitation.6 Outpatient visits for the
evaluation of GERD have increased significantly over
time.7 It is also the most common indication for EGD in
the United States.8Adverse events of GERD
Peptic strictures. The endoscopic evaluation and management of peptic strictures is discussed in another ASGE guideline.39
Barrett’s esophagus. BE is a premalignant condition in which the squamous epithelium of the distal esophagus is replaced by an abnormal columnar epithelium known as specialized intestinal metaplasia.40,41 BE is found in as many as 15% of patients undergoing EGD for GERD.42,43 Recommendations regarding the role of EGD for screening and surveillance for BE were recently published.17 The value and optimal method of screening for BE remains unclear.17 Widespread screening of the entire population with GERD would not be feasible given both the high prevalence of GERD in the Western world and the presence of many asymptomatic individuals harboring BE.44,45
SUMMARY
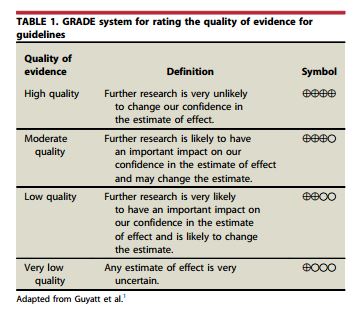
- We recommend that uncomplicated GERD be diagnosed on the basis of typical symptoms without the use of diagnostic testing, including EGD.++++
- We recommend EGD for patients who have symptoms suggesting complicated GERD or alarm symptoms. +++0
- We recommend that EGD not be routinely performed solely for the assessment of extraesophageal GERD symptoms.+++0
- We recommend that endoscopic findings of reflux esophagitis be classified according to an accepted grading scale or described in detail.+++0
- We suggest that repeat EGD be performed in patients with severe erosive esophagitis after at least an 8-week course of PPI therapy to exclude underlying BE or dysplasia.++00
- We recommend against obtaining tissue samples from endoscopically normal tissue to diagnose GERD or exclude BE in adults.+++0
- We suggest that endoscopy be considered in patients with multiple risk factors for Barrett’s esophagus. +000
- We recommend that tissue samples be obtained to confirm endoscopically suspected Barrett’s esophagus. ++++
- We suggest that endoscopic antireflux therapy be considered for selected patients with uncomplicated GERD after careful discussion with the patient regarding potential adverse effects, benefits, and other available therapeutic options.++00
Additional Resources:
(1) Guidelines For The Diagnosis and Management of Gastroesophageal Reflux Disease [PubMed Abstract] [Full Text HTML] [Full Text PDF]. Am J Gastroenterol 2013; 108:308 – 328; doi: 10.1038/ajg.2012.444; published online 19 February 2013. This is an additional resource.
(2) Gastro-oesophageal reflux disease and dyspepsia in adults: investigation and management Clinical guideline [CG184] Published date: September 2014 Last updated: November 2014
(3) Suspected cancer: recognition and referral NICE guideline [NG12] Published date: June 2015
(4) Diagnostic value of symptoms of oesophagogastric cancers in primary care: a systematic review and meta-analysis [PubMed Abstract] [Full Text HTML] [Full Text PDF]. Br J Gen Pract. 2015 Oct;65(639):e677-91. doi: 10.3399/bjgp15X686941.