Most of what follows is from Dr. Helman’s outstanding show notes of the podcast [placed here because doing that helps me put everything in my memory]:
There are many great airway podcasts and vidcasts and this blog has reviewed many of them. To review all the airway posts on the blog go to Categories and click on “Airway Management“.
Drs. Helman and Weingart’s podcast, Ep 110 Airway Pitfalls – Live from EMU 2018 [Link is to the podcast and show notes], is the best single airway podcast I’ve reviewed. And Dr. Helman’s show notes are simply the best single memory aid on airway management to me.
This is EM Cases Episode 110 – Airway Pitfalls Live from EMU 2018.
The last decade has seen a torrent of literature and expert opinion on emergency airway management. It is challenging to integrate all this new information into a seamless flow when faced with a challenging airway situation. In this live podcast recorded at North York General’s Emergency Medicine Update Conference 2018, Scott Weingart and Anton Helman put together the latest in emergency airway management by outlining 6 common airway pitfalls: Failure to prepare for failure, failure to position the patient properly, failure to optimize oxygenation, failure to optimize hemodynamics, failure to consider an awake intubation and failure to prepare for a cricothyrotomy…
I listened to the podcast several times and also reviewed the show notes which are also excellent.
The show notes contains an incredible amount of extra information. You might want to review them several times also.
The podcast starts out with a stress management tool and mneumonic: Beat (Deep Slow Breaths), The (Positive Self-Talk), Stress (See [Mental Rehearsal] Yourself Self Successfully Completing The Procedure), Fool (Focus-Use A Trigger Word [which you’re practiced] To Put Yourself In The Right Frame Of Mind).
And review Dr. Weingart’s podcast on the subject: EMCrit RACC Podcast 220 – Beat the Stress Fool with Mike Lauria — Just In Time Performance-Enhancing Psychological Skills
March 19, 2018
Dr. Weingart’s podcast has links to other related excellent resources including:
- Psychological Skills to Improve Emergency Care Providers’ Performance Under Stress [PubMed Abstract] [Full Text HTML] [Full Text PDF]. Ann Emerg Med. 2017 Dec;70(6):884-890. doi: 10.1016/j.annemergmed.2017.03.018. Epub 2017 Apr 29.
- Optimizing Crisis Resource Management to Improve Patient Safety and Team Performance: A handbook for all acute care health professionals. [Link to the free download of the PDF]. 1st. Edition May 15th, 2017 from The Royal College of Physicians and Surgeons of Canada.
What follows is from the show notes of the podcast [placed here because it helps me put everything in my memory]:
Airway Pitfall #1: Failure To Plan For Failure
ABC plans: Have a plan A, plan B if plan A fails and plan C if plan B fails.
Plan A is primary laryngoscopy – either VL or DL. A recent RCT suggests using VL with a Bougie to optimize first attempt success in anticipated difficult airways. After 3 attempts with a change in VL vs DL, position and/or intubators, move on to plan B.
Plan B is rescue with a supraglottic device (e.g. i-gel, LMA, AirQ, King LT). If the supraglottic device does not result in rapid improvement in oxygenation and end tidal CO2, declare to your team that you are in a “can’t intubate, can’t oxygenate” situation and move on to plan C – cricothyrotomy.
Plan C is cricothyrotomy
Minimal failed airway bedside gear list within arms reach:
For plan A: VL, DL, ETT, Bougie, end tidal CO2
For plan B: supraglottic airway device
For plan C: scalpel, Bougie, size 6 ETT
Drs. Weingart and Helman give an excellent discussion of the practical aspects of cricothyrotomy on the podcast from 33:15 to 37:00.
Verbalize your plan A, B and C to your team
For example: “I’m gonna take the first attempt at laryngoscopy with VL and bougie and if that fails I’m gonna try DL. If those two fail, Dr. Smith, the most experienced intubator in the room, is gonna take over. If our 3 attempts fail, we’ll place a supraglottic device, and if we can’t get a good pulse oxygenation and end-tidal CO2 witht the supraglottic device, we’re going to cut the neck.”
In this way, you’ve empowered your team to anticipate every move and to remind you if you go off plan.
This next step is one of the very critical ones (each step is critical). Always have your “push-dose epinephrine” [link is to detailed directions to preparing your push-dose syringe] prepared (ready to go) for every intubation since you never know when an apparently stable patient will crash with your RSI meds.
Prepare your pressors
Consider hanging a norepinephrine drip running at 10 micrograms/min in a large antecubital peripheral line beforesecuring the airway in all septic patients and all patients who you anticipate might drop their BP as a result of endothracheal intubation.
In addition, have “push-dose” epinephrine 10 micgrograms/mL mixed, drawn up and labeled with the concentration in the event that the BP tanks during or after intubation
Aim for a MAP of 80 or SBP of 120-140.
[And Dr. Weingart reminds us to take action – meaning give a pressor – when the blood pressure falls seriously below your goal. This is because below a certain MAP (I believe that MAP is 60 mm Hg) the heart can’t pump blood and things go very bad. So when that happens, you’re going to immediately initiate a pressor while you figure out what to do next.]
Airway Pitfall #2 Failure to Position the Patient Properly
Maintain the patient in an upright position for as long as possible prior to laying them to 20-30 degrees in order to minimize lung atelectasis and decrease work of breathing.
There are 3 elements of patient position to optimize endotracheal intubation:
- Ear to sternal notch – a line drawn from the external meatus of the ear to the sternum should be parallel with the ceiling
- Face parallel to ceiling – bring the jaw up so that the face is parallel to the ceiling
- Base of neck flexion – ensure that the base of the neck is slightly flexed
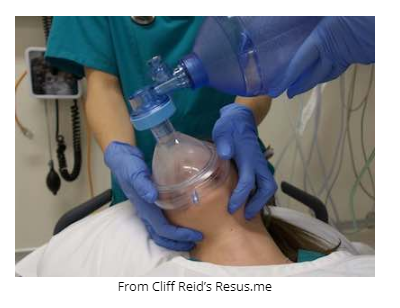
The head rotation trick for easier BVM ventilation
If you are having difficulty bagging the patient after they have been paralyzed or maintaining oxygenation and adequate end tidal CO2, besides using an oral airway and a proper two handed BVM technique, one trick is to rotate the patient’s neck about 45 degrees. This may overcome the resistance you were feeling with BVM ventilations. If this doesn’t improve things go immediately to Plan B – supraglottic device.
Cliff Reid’s post on head rotation for mask ventilation
The head lift maneuver to bring the cords into view
After you’ve positioned the patient properly as described above and you still can’t achieve a good view of the cords, consider a head lift maneuver as shown in this video care of George Kovacs and the AIME Course.
Avoid over-leavering video laryngoscope
As shown in this video and in a recent RCT, a deliberately restricted laryngeal view with the GlideScope® video laryngoscope is associated with faster and easier tracheal intubation when compared with a full glottic view. If you over-leaver the video laryngoscope it can make it difficult to place the endotracheal tube through the cords. If this happens consider pulling back a bit on the scope to give you a partial view, which may allow easier passage of a Bougie or endotracheal tube. Video care of Dr. Max Ben Yakov and Hospital for Sick Children ED Group
Airway Pitfall #3: Failure to Optimize Oxygenation
As described in EM Cases Episode 54 – Preoxygenation and Delayed Sequence Intubation, the “triple 15 rule” can help to optimize oxygenation and denitrogenation prior to intubation which may protect patients from life-threatening desaturation during endotracheal intubation. Apply at least 15L O2 via nasal prongs, plus at least 15L O2 via non-rebreather, and if oxygen saturation <95-100% then apply 15cm H2O of CPAP while maintaining nasal prongs either via bag-valve-mask with a PEEP valve, using a good mask seal over nasal prongs, or by placing the patient on CPAP, also leaving the nasal prongs on. Use up to a maximum of 15cm H2O to prevent opening the lower esophageal sphincter.
Original post on Triple 15 Rule
Airway Pitfall #4: Failure to Optimize Hemodynamics for RSI
Aim for a SBP = 120-140 or a MAP = 80 prior to intubation.
This can be achieved during the 3 stages of airway management:
- Resuscitate before you intubate – consider crystalloid with the addition of norepinephrine infusion or blood products via a large antecubital peripheral IV or rapid tranfuser depending on the particular clinical scenario.
- Induction and paralysis – for the hemodynamically precarious patient consider decreasing the sedation agent dose and increasing the paralytic agent dose to avoid a precipitous drop in BP during intubation. For example Ketamine 0.5mg/kg or 25-50mg IV in adults until the patient is dissociated and then Rocuronium 2mg/kg or 150-200mg IV in adults. Standard RSI doses of Ketamine (1-2mg/kg IV) may cause a precipitous drop in BP in those patients who are “catecholamine deplete”, and standard doses of Rocuronium (1mg/kg) in a patient in a shock state or poor cardiac output the onset of effect may take up to 4-5 minutes.
- After intubation – if the BP drops after intubation, consider the use of push dose pressors such as epinephrine drawn up prior to intubation as per this dosing.
Simplified dosing of sedation and paralytic agents in the hemodynamically compromised adult patient: Ketamine 50mg + Rocuronium 150mg
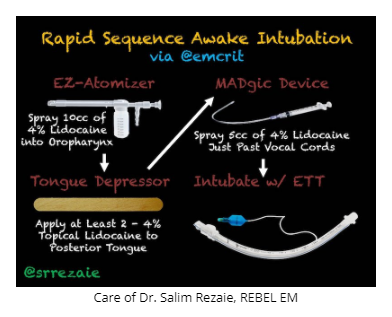
Airway Pitfall #5: Failure to Consider Awake Intubation
When to consider awake intubation
- Anticipated difficultly with ventilation (high BMI, significant facial trauma, Mallampati 4)
- Hemodynamic instability that persists despite usual pre-intubation resuscitation measures
- Poor oxygenation that persists despite employing the Triple 15 rule
- Altered airway anatomy (facial smash, epiglottitis)
- History of difficult/failed intubation
How to anesthetize for awake intubation (“topicalization”) by George Kovacs video #1
More detailed video of Airway Topicalization for an Awake Carina Selfie by Dr. Kovacs
Richard Levitan discussed airway management of morbidly obese ED patients in Episode 69
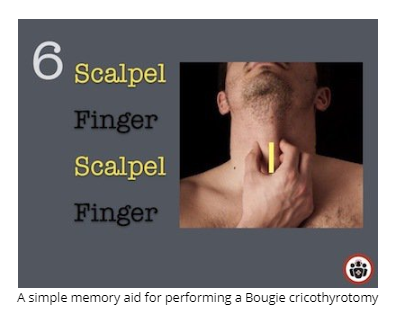
Airway Pitfall #6: Failure to Prepare for Cricothyrotomy
Surgical cricothyrotomy is indicated in “can’t intubate, can’t oxygenate scenarios”. This typically occurs after 3 failed DL and/or VL attempts followed by a failure to oxygenate adequately using a supraglottic device (Plan A, Plan B failure).
The procedure itself is not difficult. What is difficult (if you don’t prepare adequately) is the mental leap required to start doing the procedure. This psychological barrier can be overcome more easily if you prepare as outlined below.
The Difficult Airway Society guidelines recommend the scalpel-bougie technique.
Phase 1: Before you start your ED shift
- Familiarize yourself with a standardized challenging airway cart containing simple Bougie-assisted cric kit (Bougie, #10 scalpel, 6.0mm ETT).
- Establish a cohesive “difficult airway” program in your hospital based on current guidelines adapted to your specific environment.
- Two-step simulation training: low fidelity deliberate practice with simulation model followed by case-based simulation to augment psychological skills in a stressful situation.
- Post a standardized algorithm on the wall of your ED resuscitation room.
Details on Laura Duggan’s wearable cricothyrotomy trainer
Detailed anatomy on how to identify the cricothyroid membrane by Andy Neill. [I didn’t find Dr. Neill’s post that helpful. Given all the other information in these show notes that we need to master, I would skip that post.
Phase 2: Before you perform the cric
- Mark the cricothyroid membrane with an indelible marker before any intubation attempt in anticipated challenging airway scenarios. This provides you and your team confidence in starting the procedure if it becomes necessary. Consider POCUS to aid in locating the cricothyroid membrane.
- Verbalize a failed airway plan and assign roles to your team.
- Clearly announce a “can’t intubate, can’t ventilate” situation.
Scalpel-Finger-Bougie technique details on Best Case Ever 71
And again Drs. Weingart and Helman go over the cricothyrotomy technique from 33:15 to 37:00 of the podcast. Dr. Weingart says that we should not worry if we cannot palpate any anatomy (meaning we can’t detect the cricothyroid membrane before beginning the procedure. Dr. Weingart says if we can’t detect the anatomy we will make a midline incision from the top of the neck to the sternal notch. There will be blood so just keep going. We’re going to seperate the tissue with our fingers. And Dr. Weingart assures us that after we do that we will be able to palpate the thyroid cartilage, and cricoid cartilage, and the cricoid membrane.
General Airway poster for your ED by Dr. Caroline Shooner
Take Home Messages from Airway Pitfalls Live from EMU 2018
And thank you very much to Drs. Helman and Weingart for this awesome podcast.
And thank you very much to Dr. Helman for these absolutely wonderful show notes.