Resource (1), Diagnosis and Management of Ovarian Cancer published in the American Family Physician, is an outstanding review. What follows are excerpts from that article:
Abstract:
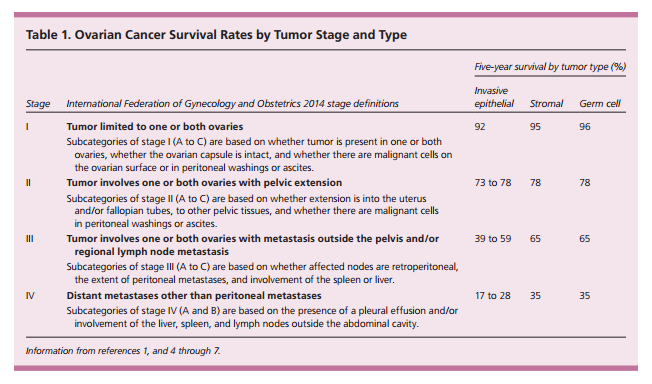
Ovarian cancer is the most lethal gynecologic cancer. Less than one-half of patients survive for more than five years after diagnosis. Ovarian cancer affects women of all ages but is most commonly diagnosed after menopause. More than 75% of affected women are diagnosed at an advanced stage because early-stage disease is usually asymptomatic and symptoms of late-stage disease are nonspecific. The strongest risk factors are advancing age and family history of ovarian and breast cancer. Women who have symptoms concerning for ovarian cancer should undergo a physical examination, transvaginal ultrasonography, and measurement of biomarkers such as cancer antigen 125. If results are suspicious for ovarian cancer, the patient should be referred to a gynecologic oncologist. Despite the low rate of early diagnosis, guidelines recommend against routine screening for ovarian cancer in average-risk women because screening, including routine pelvic examinations, is ineffective and associated with harm. However, a recent trial found a potential benefit of annual screening using an algorithm based on serial cancer antigen 125 measurements followed by transvaginal ultrasonography for women at increased risk, as determined by the algorithm. Women with an increased-risk family history should be referred for genetic counseling and, if genetic mutations (e.g., BRCA mutations) are identified, bilateral salpingo-oophorectomy can be considered for risk reduction. In both average- and high-risk women, long-term hormonal contraceptive use reduces risk by about 50%. The treatment of ovarian cancer usually involves surgery, with or without intraperitoneal and intravenous chemotherapy. Primary care physicians have important roles in posttreatment surveillance and end-of-life care. (Am Fam Physician. 2016;93(11):937-944. Copyright © 2016 American Academy of Family Physicians.)
Indications for Referral
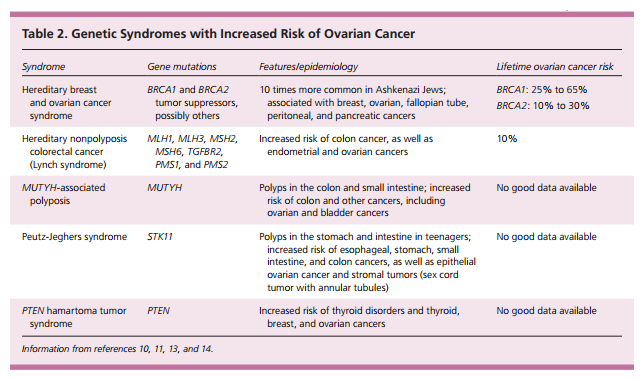
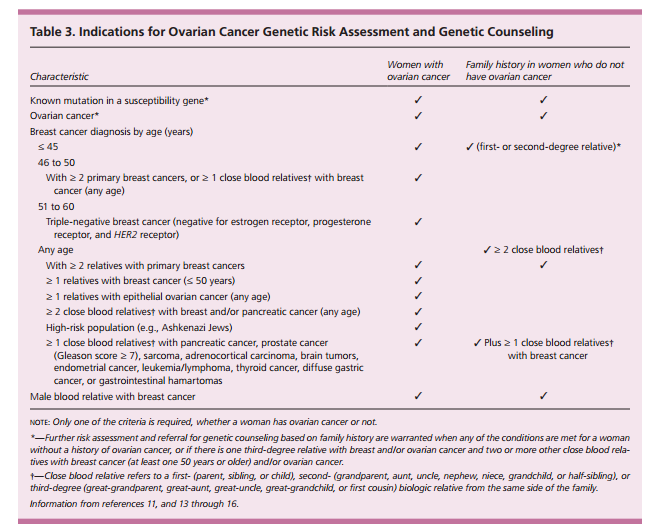
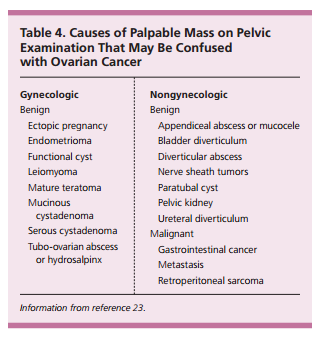
Women who have a high-risk family history should be referred for genetic testing.13,16 Women whose evaluation suggests ovarian cancer (based on imaging or laboratory test results) should be referred to a gynecologic oncologist (Figure 1). A serum CA 125 level greater than 200 U per mL (200 kU per L) in a premenopausal woman or any elevation in a postmenopausal woman, nodular or fixed pelvic masses, evidence of metastasis, or unexplained ascites are definite indications for referral. Referral to a gynecologic oncologist is also recommended for women with suspicious or complex adnexal masses on transvaginal ultrasonography that persist on short-interval (typically one to three months) follow-up imaging; premenopausal nonpregnant women with an ovarian volume greater than 20 mL; or women with ovarian volume greater than 10 mL after menopause.23
Resources:
(1) Diagnosis and Management of Ovarian Cancer [PubMed Abstract] [Full Text HTML] [Full Text PDF]. Am Fam Physician. 2016 Jun 1;93(11):937-944.
(2) Editorials
What Women and Their Physicians Need to Know About the UKCTOCS Study and Ovarian Cancer Screening [Full Text HTML] [Full Text PDF]. Am Fam Physician. 2016 Jun 1;93(11):903-904.
(3) Frequency of symptoms of ovarian cancer in women presenting to primary care clinics [PubMed Abstract] [Full Text HTML + Link To Download PDF]. JAMA. 2004 Jun 9;291(22):2705-12.
(4) Development of an ovarian cancer symptom index: possibilities for earlier detection [PubMed Abstract] [Full Text HTML] [Full Text PDF]. Cancer. 2007 Jan 15;109(2):221-7.
(4) Ovarian Cancer: A Review of Current Serum Markers and Their Clinical Applications Date: MAR.1.2013 // Source: Clinical Laboratory News
(5) The FDA recommends against using screening tests for ovarian cancer screening: FDA Safety Communication Date Issued: September 7, 2016
(6) Diagnostic Value of Serum Angiogenesis Markers in Ovarian Cancer Using Multiplex Immunoassay [PubMed Abstract] [Full Text HTML] [Download Full Text PDF] . Int J Mol Sci. 2017 Jan 10;18(1).
(7) Newly diagnosed and relapsed epithelial ovarian carcinoma: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up [Full Text PDF] Ann Oncol (2013) 24 (suppl_6): vi24-vi32. Published: 01 October 2013.