In this post, I link to and excerpt from Dr. Justin Morganstern’s First10EM’s post, Canadian Association of Radiologists Guidance on Contrast-Associated Acute Kidney Injury, June 8, 2022.
Morgenstern, J. Canadian Association of Radiologists Guidance on Contrast-Associated Acute Kidney Injury, First10EM, June 8, 2022. Available at:
https://doi.org/10.51684/FIRS.128056
All that follows is from the above resource.
The paper
Macdonald DB, Hurrell C, Costa AF, McInnes MDF, O’Malley ME, Barrett B, Brown PA, Clark EG, Hadjivassiliou A, Kirkpatrick IDC, Rempel JL, Jeon PM, Hiremath S. Canadian Association of Radiologists Guidance on Contrast Associated Acute Kidney Injury. Can Assoc Radiol J. 2022 May 24:8465371221083970. doi: 10.1177/08465371221083970. Epub ahead of print. PMID: 35608223 [free full text]
Does contrast really hurt kidneys?
There is clearly uncertainty remaining in this data, but given that every controlled study shows no harm, the bulk of the evidence suggests that this is not a clinically relevant entity. Overall, I agree with their ultimate conclusion that “the role of contrast as the cause of AKI remains unproven and the risk of contrast as a cause of AKI is likely very low.”
Is blood work required before IV contrast?
For urgent scans, they give us a very clear answer: NO.
“Any patient requiring diagnosis for urgent and/or life threatening diagnosis should not have their scan delayed for the purposes of screening.”
“When the patient is in an emergent presentation (such as suspected acute stroke, pulmonary embolism, acute aortic syndrome, bowel ischemia or perforation, and other conditions), an indicated contrast-enhanced imaging study should proceed without delay. Do not delay for eGFR and do not withhold contrast that is necessary for an accurate diagnosis of the emergent pathology.”
Again, I will emphasize that these guidelines are very clear that we should not even be considering this issue in the resuscitation bay. “When a patient is facing a life-threatening illness, indicated examinations with [iodinated contrast medium] should not be withheld for fear of CA-AKI.”
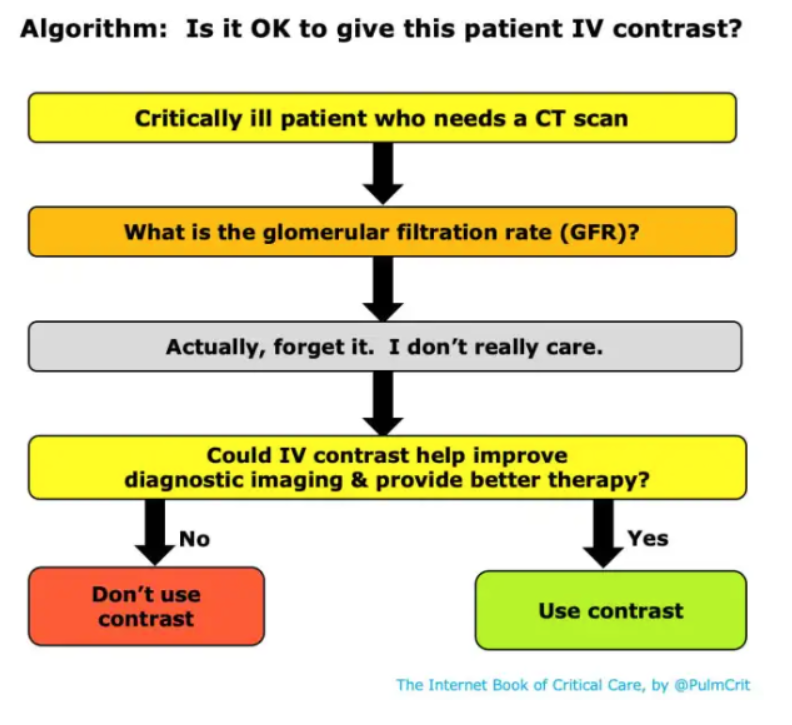
Ultimately, their recommendations essentially mirror the brilliant algorithm proposed by Josh Farkas:
If you need contrast to make an important diagnosis, you should order the test, no matter what the blood work says. Knowing that, you shouldn’t wait for blood before ordering the test, because that is just delaying the diagnosis, and potentially harming your patient.
Bottom line
These guidelines provide a reasonable summary of the evidence around IV contrast and kidney injury.
If a CT is urgent, you should never delay the CT out of consideration for renal function.
Contrast is still recommended in patients with severe chronic kidney disease or acute kidney injury if the contrast is required to make an important diagnosis and there is not a reasonable alternative diagnostic test. Therefore, if you know that a contrast CT is the only reasonable test, and you are going to order it no matter what the blood work shows, you should not delay the CT just to see the blood work results. Doing so can only hurt your patient.
The only context that blood work is reasonable prior to CT in the emergency department is if there is a reasonable alternative diagnostic test, and the delay caused by adding blood work will not result in any harm.