In this post, I link to and excerpt from Evidence Base Update for Brief, Free, and Accessible Youth Mental Health Measures [PubMed Abstract] [Full-Text HTML] [Full-Text PDF]. J Clin Child Adolesc Psychol. Jan-Feb 2020;49(1):1-17.
The above article has been cited by 4 articles listed on the Abstract page above
There is a list of 48 articles similar to the above article in the PubMed Archives.
All that follows as from the above article.
Abstract
Evidence-based assessment (EBA) is foundational to high quality mental health care for youth and is a critical component of evidence-based practice delivery, yet is underused in the community. Administration time and measure cost are barriers to use; thus, identifying and disseminating brief, free, and accessible measures is critical. This Evidence Base Update evaluates the empirical literature for brief, free, and accessible measures with psychometric support to inform research and practice with youth. A systematic review using PubMed and PsycINFO identified measures in the following domains: overall mental health, anxiety, depression, disruptive behavior, traumatic stress, disordered eating, suicidality, bipolar/mania, psychosis, and substance use. To be eligible for inclusion, measures needed to be brief (50 items or less), free, accessible, and have psychometric support for their use with youth. Eligible measures were evaluated using adapted criteria established by De Los Reyes and Langer (2018) and were classified as having excellent, good, or adequate psychometric properties. A total of 672 measures were identified; 95 (14%) met inclusion criteria. Of those, 21 (22%) were “excellent,” 34 (36%) were “good,” and 40 (42%) were “adequate.” Few measures had support for their use to routinely monitor progress in therapy. Few measures with excellent psychometric support were identified for disordered eating, suicidality, psychosis, and substance use. Future research should evaluate existing measures for use with routine progress monitoring and ease of implementation in community settings. Measure development is needed for disordered eating, suicidality, psychosis, and substance use to increase availability of brief, free, accessible, and validated measures.
Evidence-based assessment (EBA) is a cornerstone of high-quality evidence-based practice in mental health care (Hunsley & Mash, 2018; Jensen-Doss, 2011; Youngstrom et al., 2017). EBA serves two key clinical functions. First, early in treatment, EBA is essential for guiding initial case conceptualization, supporting the identification of appropriate treatment targets, and guiding clinicians in the selection of evidence-based treatment strategies (Youngstrom, Choukas-Bradley, Calhoun, & Jensen-Doss, 2015). Second, after the initial assessment, EBA guides the monitoring of treatment progress and informs the personalization of treatment to optimize treatment success (Ng & Weisz, 2016; Youngstrom et al., 2015). Use of EBA both early in treatment and throughout the course of treatment (also referred to as measurement-based care; Scott & Lewis, 2015) has been associated with improved youth treatment engagement (Klein, Lavigne, & Seshadri, 2010; Pogge et al., 2001) and youth treatment response (Bickman, Kelley, Breda, de Andrade, & Riemer, 2011; Eisen, Dickey, & Sederer, 2000; Jensen-Doss & Weisz, 2008).
Despite the promise of EBA in usual care for youth, use is low (Jensen-Doss & Hawley, 2010; Jensen-Doss, Becker-Haimes, et al., 2018; Whiteside, Sattler, Hathaway, & Douglas, 2016; Lyon, Dorsey, Pullmann, Silbaugh-Cowdin, & Berliner, 2015). Although multiple barriers to EBA exist (Boswell, Kraus, Miller, & Lambert 2015), surveys of practicing clinicians routinely demonstrate that the time and cost associated with engaging in EBA are most prohibitive (Kotte et al., 2016; Whiteside et al., 2016).
Brief, free, accessible, and validated measures to be used in EBA with youth can facilitate EBA adoption and uptake. Beidas and colleagues (2015) conducted a review of such measures for prevalent youth mental health disorders (overall mental health, anxiety, depression, disruptive behavior, eating, bipolar, suicidality, and traumatic stress).
. . . ; in the past several years, new measures may have been developed to match updated diagnostic criteria and new diagnostic categories (e.g., avoidant/restrictive food intake, disruptive mood dysregulation disorder). Finally, the original review did not include any measures related to assessment of substance use. Given the growing public health crisis related to substance abuse in adolescence (Degenhardt et al., 2016), it is important to extend the initial review to cover measures of youth substance use.
This systematic review provides a comprehensive Evidence Base Update for brief, free, and accessible EBA measures for use in youth mental health, guided by criteria set forth by De Los Reyes and Langer (2018; see Table 1).
Measure Eligibility
Measures were required to meet four inclusion criteria to be eligible. Specifically, measures had to: 1) be brief (i.e., defined as 50 items or fewer, including sub-items), 2) be free (i.e., no associated cost for individual use), 3) be accessible (i.e., easily obtainable in ready-to-use format on the Internet), and 4) have available data for their psychometric properties for youth. To meet the “free” criterion, measures must have included a statement that the measure was available for individual use without charge.
Results
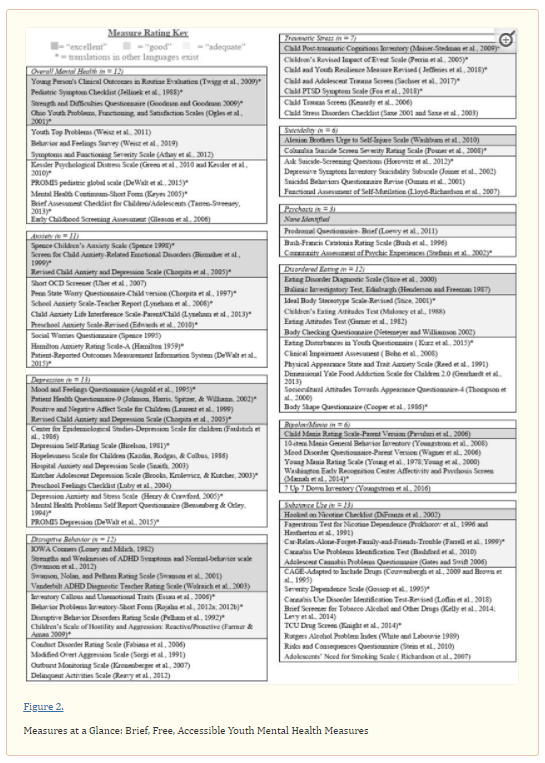
Supplemental tables 1–10 display the following information for all identified measures: overall psychometric rating (i.e., excellent, good, or adequate), number of items, available forms (self, parent, clinician, or teacher report), intended age range for use, intended clinical use (screening, diagnostic aid/treatment planning, or progress monitoring), evidence of treatment sensitivity, and a link to the measure.* We also denote which measures have freely available translations in other languages. Figure 2 illustrates an overview of all identified measures. A brief summary of the findings is below, by diagnostic category.
*Each of the measures shown in Figure 2 can be directly accessed by downloading Supplemental tables 1-10.