Watching out for an inappropriate tachycardia or tachypnea can alert you to a potentially serious problem perhaps before the patient appears obviously toxic. The excerpt below tells you how to determine an inappropriate pediatric tachycardia or tachypnea.
See Pediatric Fever – A Link To A Great Podcast Review From Emergency Medicine Cases Posted on January 30, 2016 by Tom Wade MD:
Here are some excerpts from the show notes of Episode 48 – Pediatric Fever Without A Source , July 2019, from Emergency Medicine Cases:
The value of treating the fever in the ED besides patient comfort and minimizing dehydration, is so that the child can be re-examined when afebrile to help risk stratify for SBI and to counsel the parents. If the child’s vital signs and clinical picture continue to be worrisome after their fever has been corrected, then SBI should be suspected. However, if, after normalizing the temperature, the child has normal vital signs and is clinically ‘well’, then SBI is less likely and the parents can be reassured that fever itself is not dangerous.
Temperature Corrected Heart Rate and Respiratory Rate
Heart Rate increases by approx 10 beats/min and Respiratory Rate by 5 breaths/min for every Celsius degree (1.8 degree of Fahrenheit) of fever >38°C.
For example, if the temperature is 40°C and HR 144 -> subtract 2×10 -> corrected HR 124
If the child has tachycardia after being corrected for fever, consider other contributors (pain, crying, early compensated shock). Check perfusion, ask about urine output, and have a high degree of suspicion for dehydration and sepsis.
And the same is true if there is a tachypnea after correcting for tachypnea.
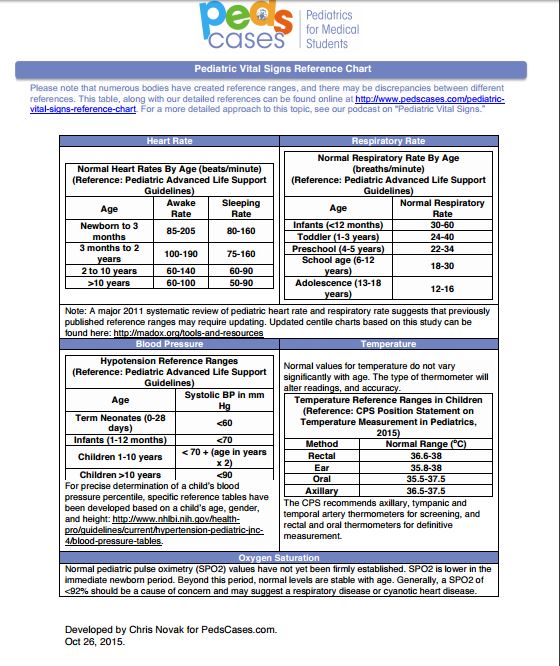
Pediatric Vital Signs Reference Chart from PedsCases – Pediatrics For Medical Students: