The following is my notes on the first of three vidcasts that are from the Essentials of Emergency Medicine 2016 Conference.
Links to Part 2 and Part 3 are below in Resources (1) and (2) in Resources at the end of today’s notes.
Low-Risk Chest Pain ADP SHOWDOWN (Using TIMI vs HEART): Pt. 1 of 3 – HEART
Dr. Rezaie uses the HEART Score for low risk patients in the Emergency Department. He states that the TIMI score is not useful in this population.
See Resource (6) below for a copy of the HEART Score. And see Resource (3) for the article on the HEART score
Dr. Rezaie did a review of 13 trials [not published at the time of this talk] and found that for a score of 0-3:
Dr. Rezaie warns us that not all of the HEART low risk score patients are actually low risk. It is very possible for a patient to have all of his HEART risk factors as negative except for his troponin.
That patient might have his troponin elevated 1 -3x or greater than 3x elevated. That patient is not low risk, Dr. Rezaie states. That patient has something that is causing them to leak troponin. Maybe it is an ACS, maybe a PE, maybe a dissection. They’ve got something going on and that is not a low risk patient that Dr. R is sending home.
What about dynamic ekg changes?
If there are dynamic ekg changes [NSST changes, ST depression] that is not a low risk patient in my mind either.
You have to be smarter than the HEART score [by paying a lot of attention to troponin and ekg changes and not just to the total point score].
So Dr. R found that about 50% of patients had a HEART score of 0 – 3 and that identified approx 50% of patients as low risk and those patients had a 30 – 45 d MACE rate of 2.7% (this is higher than the oft quoted 1.7% rate).
So Dr. Rezaie asks if there is a way we can do better that 2.7%. And his answer is YES. He cites a study where they drew a second troponin at 3 hrs and the results were:
Dr. Raziae points out that this study did not use the new high sensitivity troponins as they were not available in the U.S. at the time of the above study and Dr. Riziae’s talk although they have been available in Europe for approximately seven years.
Early this year, 2017 a high sensitivity troponin assay was approved in the U.S. Please see Resource (4).
See Resource (5) below which is a link to Dr. Raziae’s post, Management and Disposition of Low Risk Chest Pain, from his blog RebelEM. The post is basically the notes of this talk expanded.
And finally, Dr. Riziae goes over Evidence Based Medicine again (he discussed it earlier in his talk0. And here is the diagram from his talk:
 So it is very important to involve the patient in the decision making. Dr. Riziae tells his low risk patient (0-3 HEART Score with negative troponin at 1 and 3 hours and no dynamic ekg changes which turn out to be about 25% of chest pain patients):
So it is very important to involve the patient in the decision making. Dr. Riziae tells his low risk patient (0-3 HEART Score with negative troponin at 1 and 3 hours and no dynamic ekg changes which turn out to be about 25% of chest pain patients):
What I’m starting to tell my patients now is that for every 100 patients that come in in your situation. . . one in a 100 or 0.8% may have a cardiac event in the next thirty days. So let’s talk about what our options are:
Option one is I can keep you [and] we can do a stress test in the morning.
Option two is I can let you follow up with your primary care doctor and follow up the chest pain as an outpatient. Or if you don’t have a primary care doctor, I have a clinic that I can get you arranged for to have follow up for this.
Most people choose to go home as they can live with that 0.8% risk. But you must document the coversation in the medical record.
Resources:
(1) Low-Risk Chest Pain ADP SHOWDOWN (Using TIMI vs HEART): Part 2 of 3 – TIMI
(2) Low-Risk Chest Pain ADP SHOWDOWN: Part 3 of 3 – Delta Troponins and Stress Tests
(3) Chest pain in the emergency room: value of the HEART score [PubMed Abstract] [Full Text HTML] [Full Text PDF]
(4) US Debut of ‘High-Sensitivity’ Troponin Assay Signals Sea Change in Acute MI Patrice Wendling, January 25, 2017 from Medscape.com.
(5) Management and Disposition of Low Risk Chest Pain by Dr. Raziae of RebelEM and the lecturer of the above video.
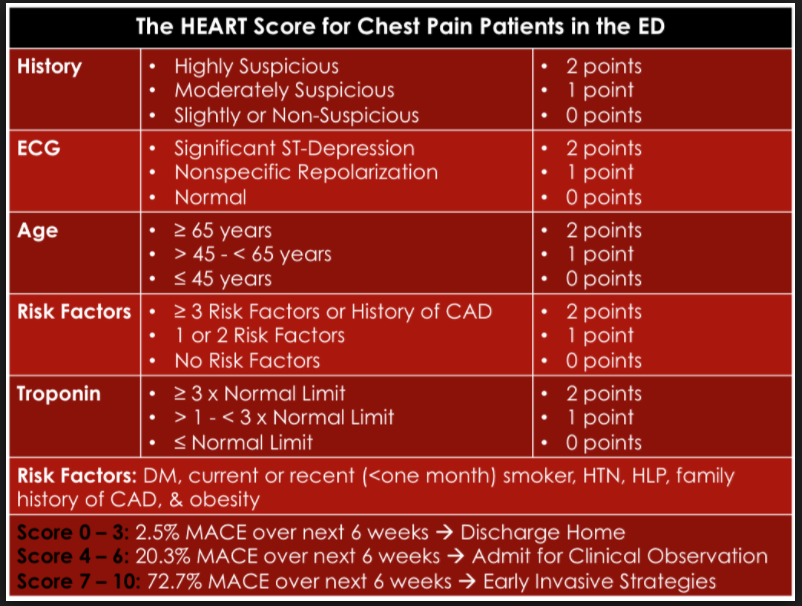
(6) The Heart Score For Chest Pain Patients In the ED. Graphic from RebelEM.com via Google Images: