Earlier this month I linked to Episode 5 – Mobile Integrated Health/Community Paramedicine Featuring Dr. Peter Antevy From MCHC Paramedic Podcast With An Additional Article, posted on March 16, 2019 by Tom Wade MD. In the podcast, Dr. Antevy discusses a new Emergency Medical Services model. The post has links to his great podcast on the subject and contains an article that introduces the subject.
For the very latest on Mobile Integrated Healthcare/Community Paramedicine see Mobile Integrated Healthcare from The Journal Of Emergency Medical Services (JEMS) And see also MOBILE INTEGRATED HEALTHCARE NEWS also from JEMS.
What follows is an additional link on the subject.
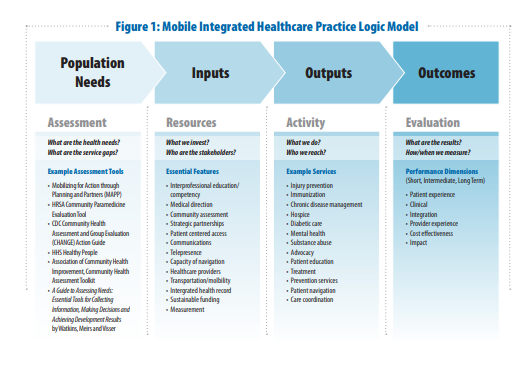
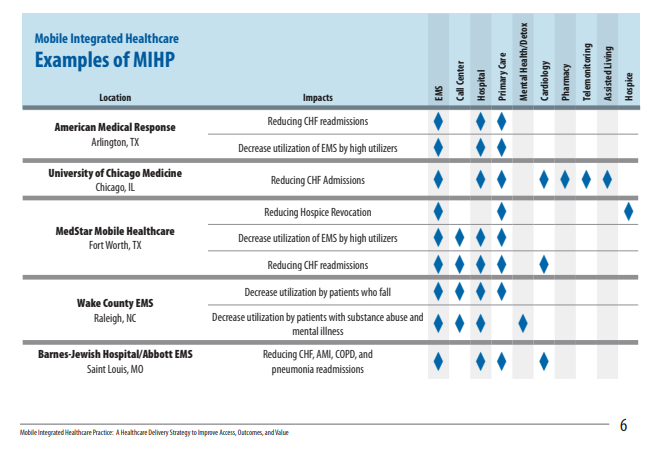
Mobile Integrated Healthcare Practice: A Healthcare Delivery Strategy to Improve Access, Outcomes, and Value [PDF] – This is an undated paper probably published around 2012. Nonetheless it provides a good introduction to the subject. Here are some excerpts:
MIHP is proposed as a restructuring of care, not a new way to spend additional health care money. In fact, most experimental initiatives in mobile care arena have demonstrated a consistent inability to establish economic sustainability because they
operate as “additions” to health care spending. In contrast, the MIHP strategy is designed tosupport and augment other patient-centered delivery models including the Patient Centered
Medical Home, the Chronic Care Model and the Accountable Care Organization by providing an optimized mix of care, likely at costs lower than traditional models. In most cases, it is likely
that MIHP could be funded within one of these models as a cost-optimization strategy based on shared savings.The essence of the MIHP strategy is that each MIHP program will be unique, defined by local gap analysis and population needs assessment. This process is well validated in public health,[6] and many evidence-based tools are now available to assess local area health care needs, infrastructure and resources.[7-9] Population assessments should be informed by the analysis
of health data on specific known health or social issues, by identified gaps in current services, and the insights of stakeholders, including patients and their families.After considering the range of existing mobile health assets, we conclude that the most common existing mobile health care system—the Emergency Medical Services (EMS) system—is
well suited to host the MIHP and coordinate service delivery by multiple providers.