I recently completed the International Trauma Life Support Course (ITLS) at IU Health Methodist Hospital in Indianapolis. It was an excellent course and I believe that any clinician interested in trauma care will benefit from it.
This blog is basically my study notes and my peripheral brain. Placing my notes online makes makes them available to me anywhere. And that is because the excellent built-in search function of the content management software [WordPress] makes it easy to find my notes on any topic when I want to review them.
This post contains excerpts from International Trauma Life Support For Emergency Care Providers Provider Manual, 2016*.
* Here are links to:
Specifically, this post consists of excerpts from Chapter 3 Assessment Skills, p 50 – xx .
Assessment Skills:
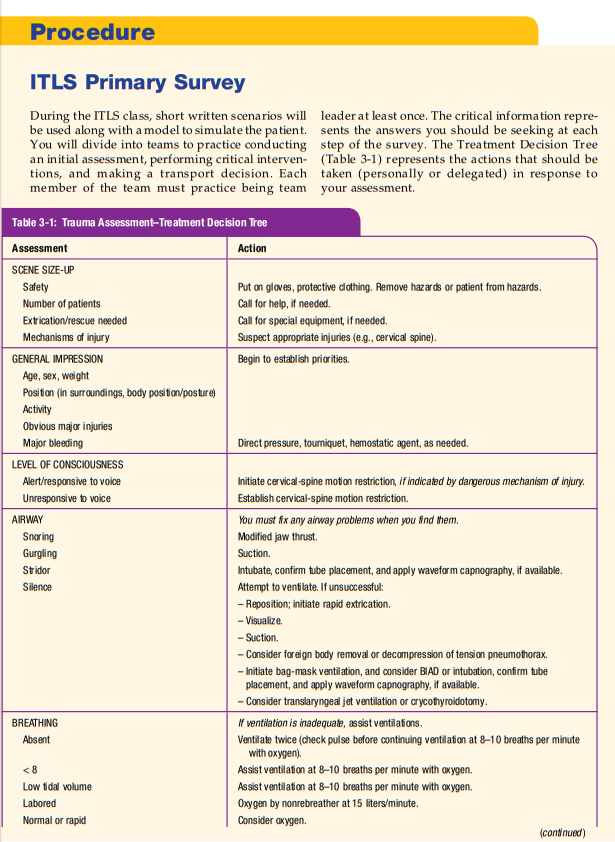
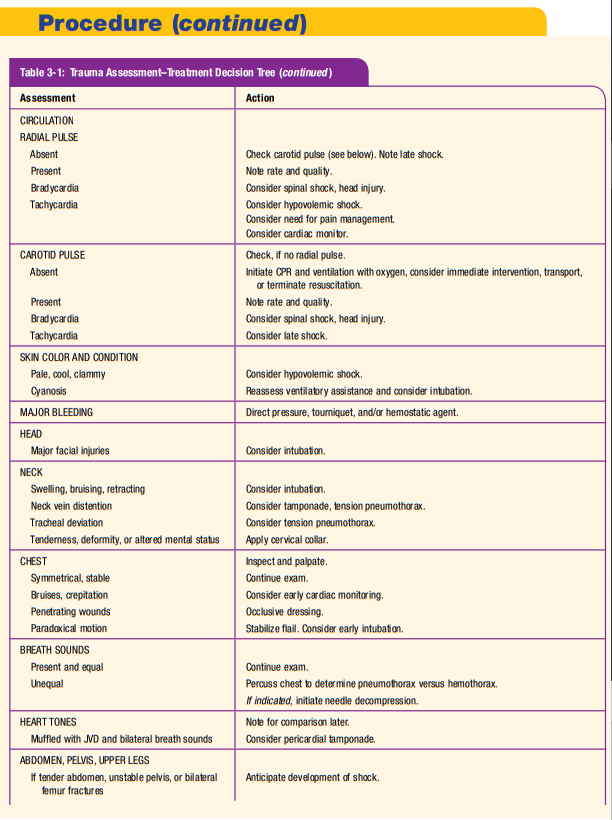
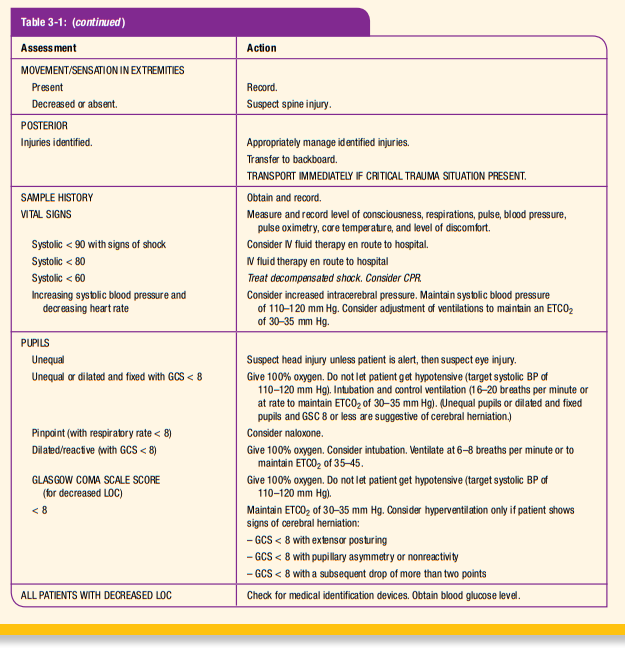
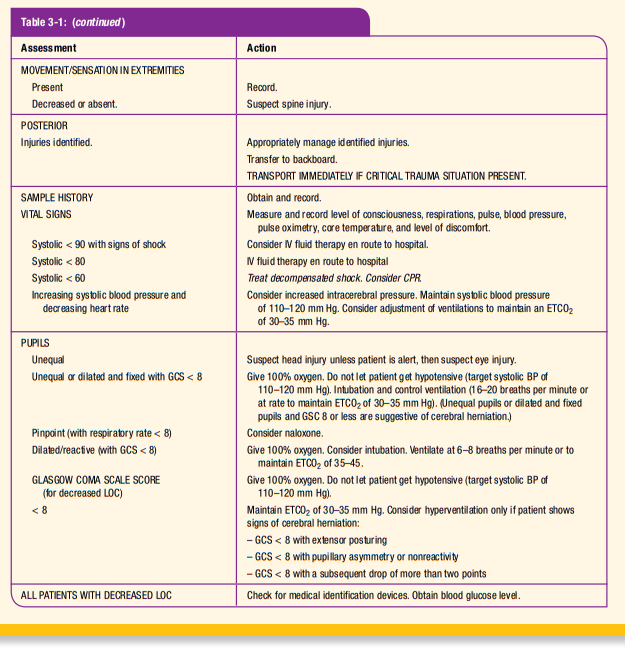
ITLS Primary Survey—Critical Information
If you ask the right questions, you will get the information you need to make the critical decisions necessary in the management of your patient. The following questions are presented in the order in which you should ask yourself as you perform the
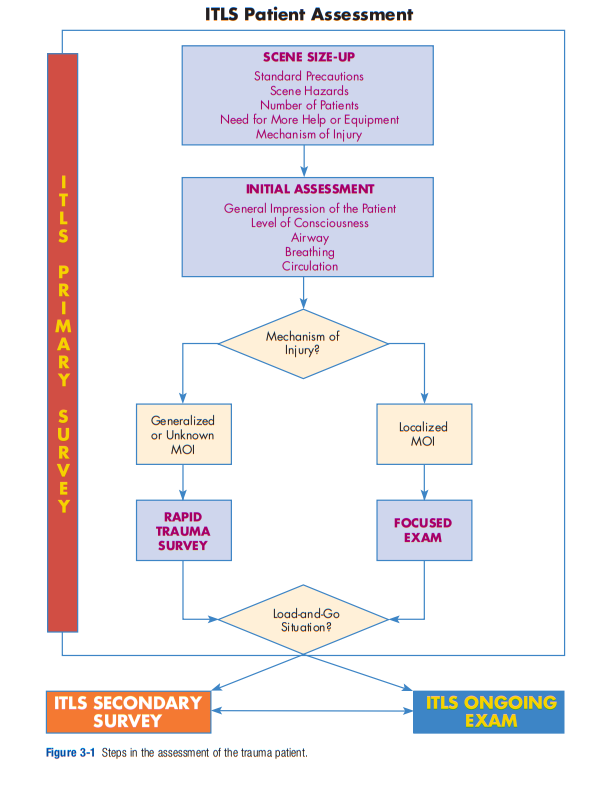
ITLS Primary Survey. This is the minimum information that you will need as you perform each step of the ITLS Primary Survey (Figure 3-1):
Scene Size-up
• Have I taken standard precautions?
• Do I see, hear, smell, or sense anything dangerous?
• Are there any other patients?
• Are additional personnel or resources needed?
• Do we need special equipment?
• What is the mechanism of injury here?
• Is it generalized or focused?
• Is it potentially life threatening?
Initial AssessmentGeneral Impression
• What is my general impression of the patient as I approach?
• Is there obvious life-threatening external bleeding that must be addressed now?Level of Consciousness (AVPU)
• Introduce yourself, and say: “We are here to help you. Can you tell us what happened?”
• From the patient’s response, what is the AVPU (alert, voice, pain, unresponsive) rating?Airway
• Is the airway open and clear?
• Do I hear abnormal sounds such as snoring, gurgling, or stridor?Breathing
• Is the patient breathing?
• What is the rate and depth of respiration?
• Is breathing labored?Circulation
• Is there life-threatening external bleeding?
• What is the rate and quality of the pulse at the neck and wrist?
• What are the skin color, condition, and temperature?Decision
• Is this a critical situation?
• Is spinal motion restriction indicated?
• Does the mechanism of injury or any initial assessment findings indicate the need for a rapid trauma survey?PEARLS ITLS Primary Survey
• Do not approach the patient until you have performed a scene size-up.
• Do not interrupt the ITLS Primary Survey except for immediate threats to life such as airway obstruction, cardiac
arrest, severe hemorrhage, or if the scene becomes too dangerous. Team members may perform the necessary critical interventions while you complete the ITLS Primary Survey.
• Give any ventilation instructions as soon as you assess airway and breathing.
• Prophylactic hyperventilation is not recommended for
patients with decreased level of consciousness. Use it only for head-injury patients who show signs of the cerebral herniation
syndrome.
• Assist ventilations in anyone who is hypoventilating (less than eight breaths per minute, moving little or no air, or ETCO2 of greater than 45). Confirm adequate tidal volume based on chest rise and fall.
• Give oxygen to all multipletrauma patients. If in doubt or a pulse oximeter reading of less than 95 is present, give oxygen.
• Endotracheal tubes are the best method to protect the airway
and provide ventilatory assistance to the adult patient. Other methods may be effective but are not as secure.
• If spinal motion restriction (SMR) is indicated, transfer the patient to the backboard as soon as the ITLS Primary Survey is completed.
• When the ITLS Primary Survey is completed, decide if the patient is critical or stable.
• Communicate with medical direction and the receiving facility early if you have a critical patient.
• If the patient has a critical trauma situation, load him or
her into the ambulance and begin transport. (Transport the pregnant patient tilted slightly to the left.)
• If absolutely necessary, certain critical interventions may have
to be done before transport. Remember that you are trading
minutes of the patient’s Golden Period for those procedures.
Use good judgment. They may include establishing an airway,
ventilation, oxygen administration, control of serious external
bleeding, sealing an open pneumothorax, decompression of a tension pneumothorax, stabilization of impaled objects, and packaging (with SMR when indicated) thepatient for transport.
• For patients in traumatic cardiac arrest, address treatable causes and then determine whether to continue the resuscitation.
• The indications to decompress a tension pneumothorax include signs of a tension pneumothorax and more than one of the following: respiratory distress and cyanosis, loss
of radial pulse (obvious shock), loss of consciousness, or an
obviously decreasing level of consciousness.
• Unless the patient is entrapped or the ambulance has not
arrived on scene, start intravenous therapy while transporting the patient to the receiving facility.Rapid Trauma Survey
(See Figure 3-2.)
Head and Neck
• Are there obvious wounds of the head or neck?
• Is there deformity or tenderness of the neck?
• Are the neck veins distended?
• Does the trachea look and feel midline or deviated?Chest
Start here on p 57