In this post I link to and excerpt from The Telehealth Ten: A Guide for a Patient-Assisted Virtual Physical Examination [PubMed Citation] [Full-Text HTML] [Full-Text PDF]. Am J Med. 2021 Jan; 134(1): 48–51. Published online 2020 Jul 18. doi: 10.1016/j.amjmed.2020.06.015
The above article has been cited by 11 articles in PubMed.
There are 123 similar articles available in PubMed. Many are free PMC articles. All telehealth practioners should review this outstanding list of articles.
The above article has been commented on in
-
A Few More Findings on the Inspection of Cardiovascular System in Telehealth.
Am J Med. 2021 Feb;134(2):e139. doi: 10.1016/j.amjmed.2020.08.025.PMID: 33551048 No abstract available. -
Am J Med. 2021 Feb;134(2):e140. doi: 10.1016/j.amjmed.2020.09.009.PMID: 33551049 No abstract available.
-
The Novel Concept of Patient Self-Imaging: Success in COVID-19 and Cardiopulmonary Disorders.
Am J Med. 2021 May;134(5):e360-e361. doi: 10.1016/j.amjmed.2021.01.010.PMID: 33962720 Free PMC article. No abstract available.
All that follows is from The Telehealth Ten: A Guide for a Patient-Assisted Virtual Physical Examination [PubMed Citation] [Full-Text HTML] [Full-Text PDF]. Am J Med. 2021 Jan; 134(1): 48–51. Published online 2020 Jul 18. doi: 10.1016/j.amjmed.2020.06.015.
Introduction
“The only problem with communication is the assumption it occurred.”
George Bernard Shaw
Listening to patients’ stories is an essential clinical skill.
When combined with caring and clinical expertise, patients
report confidence in clinicians with strong communication
skills.1 Given the coronavirus disease 2019 (COVID-19)
pandemic and the need to keep vulnerable patients (and
clinicians) at home and away from health care facilities to
decrease risk of virus transmission, there has been a rapid
increase in use of virtual, or telehealth, visits.2 A new reliance on telehealth requires many clinicians to develop skills
to obtain objective information from these types of visits.3
Although eliciting a complete history and adjudicating
medication lists and allergies are foundational activities of
virtual visits, additional information from a telehealth physical examination can be useful. A targeted physical examination either confirms clues suggested by the history or
provides data that can direct specific clinical tests or treatments. Our experience is that patients respond positively to
these maneuvers. Thus, performance of a telehealth physical examination may be considered as an essential element
in the context of postpandemic payment policies for telehealth visits.Astute physicians start the physical examination as the
patient walks into the room because this provides immediate clues about patients’ characteristics. Observing the patient’s gait and level of effort to walk into the room and to sit up on the examination table can be useful to assess his or her functional performance. How can clinicians obtain this and other similar information in a telehealth visit?Use of virtual visits requires physicians to think proactively about what information they wish to obtain from the
examination that can be performed remotely. While video
can provide visual clues that one may also obtain on an inperson examination, it is possible to elicit additional valuable clinical information through various patient-assisted
maneuvers. Thus, a trained clinician can purposefully facilitate the focused clinical examination by directly asking the
patient, his or her caregiver, or both, a set of questions. This
evaluation can be enhanced using digital devices such as
wearables for heart rate and electrocardiogram, and home
monitoring devices (scale, blood pressure cuff, and pulse
oximeter), which are potentially available to patients. We
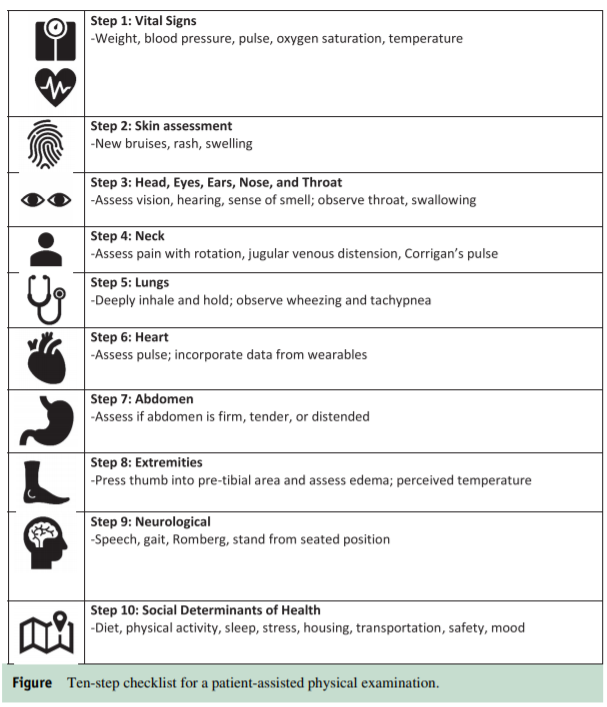
propose the “Telehealth Ten,” which is a patient-assisted
clinical examination to help guide clinicians through this
new territory (Figure). This is not a comprehensive list, but
focused primarily for chronic disease patients with an
emphasis on cardiovascular disease management.
Please note that the list of similar articles, citations, and comments at the beginning of this post has many suggestions on enhancing the various aspects of the telehealth exam.
TEN STEPS FOR A PATIENT-ASSISTED VIRTUAL
PHYSICAL EXAMINATION