In this post I link to and excerpt from Dr Josh Farkas’ chapter, Acute Pancreatitis [Link is to the podcast] [Link is to the show notes], of November 23, 2016.
Note to readers: The best place for you to review Dr. Farkas’ Acute Pancreatitis are the links above. I only excerpt from them because doing so helps me retain the material and I can find the topic more quickly using my blog’s categories and search functions.
Dr. Farkas writes in his introduction:
Management of severe pancreatitis has remained in a state of controlled chaos and persistent debate for years (mirroring evolution in our treatment of septic shock). This confusion shows no signs of abating in the near future. This chapter explores a reasonable approach to pancreatitis, with the caveat that there is very little evidence available to guide our combat against this challenging foe.
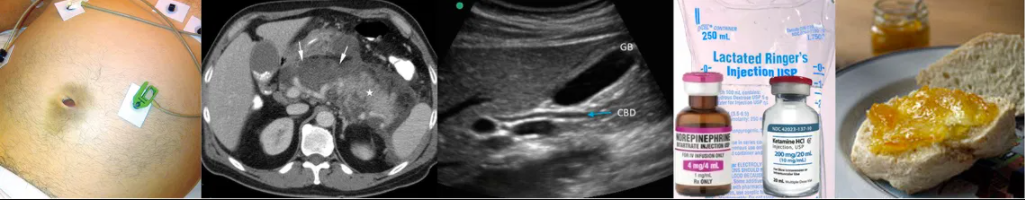
Here is the graphic from the chapter:
Here are the direct links that Dr. Farkas provides to each section of his chapter:
CONTENTS
And here are excerpts from this outstanding chapter:
diagnosis
diagnostic criteria for acute pancreatitis
- At least two of the following are required:
- (1) Elevation of lipase >3 times upper limit normal (1)
- (2) Characteristic abdominal pain
- (3) Imaging evidence of pancreatitis on CT, MRI, or ultrasound.
- Patients not meeting these criteria don’t have pancreatitis and should not be treated for it.
clinical findings
- Pain:
- Typically in epigastrum or left upper-quadrant, may radiate to back.
- Epigastric tenderness on exam is usually present.
- Persistent nausea/vomiting
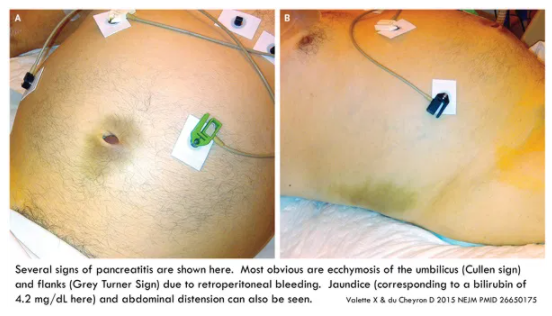
- Hemorrhagic pancreatitis may cause Cullen Sign & Grey Turner Sign:
lipase
- Sensitivity and specificity ~90% for acute pancreatitis.
- Causes of elevated lipase include:
- Pancreatic disease of any sort (pancreatitis, pseudocyst, cancer)
- Intestinal obstruction/pseudo-obstruction, perforation, duodenal ulceration, ischemia
- Biliary disease (cholecystitis, cholangitis, choledocholithiasis)
- Renal failure
- Elevations of lipase due to diseases other than pancreatitis tend to be under three times the upper-limit normal.
- Very high lipase values are more specific for a diagnosis of pancreatitis.
- Higher lipase values don’t correlate with worse prognostic outcome. So severely elevated lipase values may seem scary, but they shouldn’t actually be.
- Lipase has replaced amylase for the diagnosis of pancreatitis. There is no point in checking an amylase level.
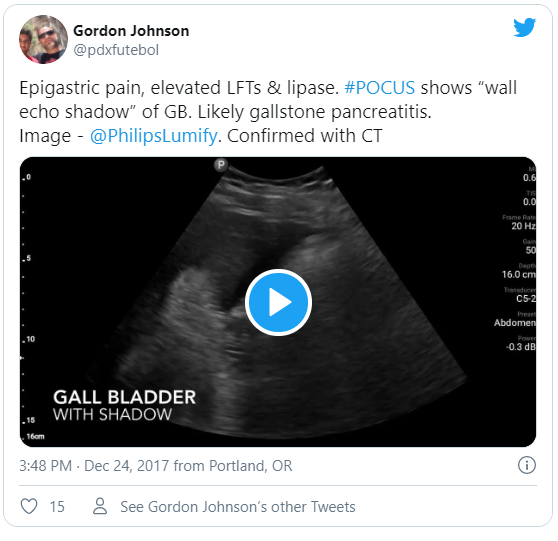
[Note: the figure below is just an image (non-functional). It is possible to embed the tweet in a post, I just don’t know how to do it right now. Here is the direct link to the tweet.]
CT scan
- Early CT if necessary to clarify the diagnosis
- CT is sensitive and specific for pancreatitis, also providing information about severity.
- If the patient definitely has pancreatitis (based on typical history, exam, and labs), then there is no reason to get an early CT scan (it won’t affect management).
- For patients in shock, CT scan is often sensible to exclude a focus of intra-abdominal sepsis.
- Late CT scan for complications
- The real role of CT scan in pancreatitis is to look for complications if the patient deteriorates later on in their course (after several days). For example, CT scan may help evaluate for infected necrosis and pseudocyst.
evaluating the cause of pancreatitis
- Gallstones (~40%)1
- Alcoholism (~30%)
- Metabolic abnormalities: hypertriglyceridemia, hypercalcemia
- Medications include:2
- antibiotics: tetracyclines, sulfonamides, pentamidine, HIV medications, isoniazid, metronidazole
- immunosuppressives: azathioprine, sulfasalazine, aminosalicylates, 6-mercaptopurine
- cardiac: amiodarone, losartan, furosemide, pravastatin, simvastatin
- valproic acid
- all-trans-retionic acid (ATRA)
- Cystic fibrosis
- Posterior penetrating ulcer, trauma
- Iatrogenic: ERCP, surgery, radiation therapy, post CABG
- Pancreatic malignancy
labs
Start here.